Abstract
Background
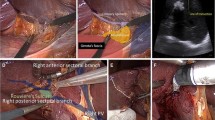
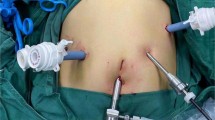
Although laparoscopic liver resection (LLR) is now considered a standard procedure in peripheral segments, there are few reports on laparoscopic segment 1 (Sg1) resection. The aim of this study was to assess both safety and feasibility of Sg1 LLR.
Methods
From 2000 to 2014, all patients who underwent LLR were identified from a prospective database. Patients with resection of Sg1 (Sg1 group) were compared with those with resection of anteroinferior segments (AI group: segments 3, 4b, 5, 6) or posterosuperior segments (PS group: segments 4a, 7, 8), in terms of tumor characteristics, surgical treatment, and short-term outcomes.
Results
There were 15, 151, and 67 patients in Sg1, AI, and PS groups. Tumor size and tumor number were similar between the three groups (p = 0.139, p = 0.102). Operative time was significantly shorter in Sg1 (150 min) and AI group (135 min) compared with PS group (180 min) (p = 0.021). Median blood loss was notably higher in PS group (140 ml) compared with Sg1 group (75 ml) and AI group (10 ml) (p = 0.001). No mortality was observed in all groups. Postoperative complication rate was 20.0 % with Sg1 group, 14.6 % with AI group, and 20.9 % with PS group (p = 0.060). The rate of major complication was significantly higher in Sg1 group (13.3 %) and PS group (11.9 %) compared with AI group (4.0 %) (p = 0.042). Resection margins were clear in all Sg1 and PS group patients, whereas two (1.3 %) patients in AI group had R1 margins (p = 0.586).
Conclusion
The laparoscopic approach of isolated resection located in the caudate lobe is a feasible and curative surgical option in selected patients.
Similar content being viewed by others
References
Kumon M (1985) Anatomy of the caudate lobe with special reference to portal vein and bile duct. Acta Hepatol Jap 26:1193–1199
Kosuge T, Yamamoto J, Takayama T, Shimada K, Yamasaki S, Makuuchi M, Hasegawa H (1994) An isolated, complete resection of the caudate lobe, including the paracaval portion, for hepatocellular carcinoma. Arch Surg 129:280–284
Dulucq JL, Wintringer P, Stabilini C, Mahajna A (2006) Isolated laparoscopic resection of the hepatic caudate lobe: surgical technique and a report of 2 cases. Surg Laparosc Endosc Percut Tech 16:32–35
Kokkalera U, Ghellai A, Vandermeer TJ (2007) Laparoscopic hepatic caudate lobectomy. J Laparoendosc Adv Surg Tech A 17:36–38
Nomi T, Fuks D, Govindasamy M, Mal F, Nakajima Y, Gayet B (2015) Risk factors for complications after laparoscopic major hepatectomy. Br J Surg 102:254–260
Nomi T, Fuks D, Kawaguchi Y, Mal F, Nakajima Y, Gayet B (2015) Learning curve for laparoscopic major hepatectomy. Br J Surg 102:796–804
Araki K, Conrad C, Ogiso S, Kuwano H, Gayet B (2014) Intraoperative ultrasonography of laparoscopic hepatectomy: key technique for safe liver transection. J Am Coll Surg 218:e37–e41
Ishizawa T, Gumbs AA, Kokudo N, Gayet B (2012) Laparoscopic segmentectomy of the liver: from segment I to VIII. Ann Surg 256:959–964
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Balzan S, Belghiti J, Farges O, Ogata S, Sauvanet A, Delefosse D, Durand F (2005) The “50–50 criteria” on postoperative day 5: an accurate predictor of liver failure and death after hepatectomy. Ann Surg 242:824–828, discussion 828–829
Koch M, Garden OJ, Padbury R, Rahbari NN, Adam R, Capussotti L, Fan ST, Yokoyama Y, Crawford M, Makuuchi M, Christophi C, Banting S, Brooke-Smith M, Usatoff V, Nagino M, Maddern G, Hugh TJ, Vauthey JN, Greig P, Rees M, Nimura Y, Figueras J, DeMatteo RP, Buchler MW, Weitz J (2011) Bile leakage after hepatobiliary and pancreatic surgery: a definition and grading of severity by the International Study Group of Liver Surgery. Surgery 149:680–688
Yanaga K, Matsumata T, Hayashi H, Shimada M, Urata K, Sugimachi K (1994) Isolated hepatic caudate lobectomy. Surgery 115:757–761
Yoon YS, Han HS, Cho JY, Kim JH, Kwon Y (2013) Laparoscopic liver resection for centrally located tumors close to the hilum, major hepatic veins, or inferior vena cava. Surgery 153:502–509
Huang MT, Lee WJ, Wang W, Wei PL, Chen RJ (2003) Hand-assisted laparoscopic hepatectomy for solid tumor in the posterior portion of the right lobe: initial experience. Ann Surg 238:674–679
Yoon YS, Han HS, Cho JY, Ahn KS (2010) Total laparoscopic liver resection for hepatocellular carcinoma located in all segments of the liver. Surg Endosc 24:1630–1637
Ogiso S, Conrad C, Araki K, Nomi T, Anil Z, Gayet B (2015) Laparoscopic transabdominal with transdiaphragmatic access improves resection of difficult posterosuperior liver lesions. Ann Surg 262:358–365
Wakabayashi G, Cherqui D, Geller DA, Han HS, Kaneko H, Buell JF (2014) Laparoscopic hepatectomy is theoretically better than open hepatectomy: preparing for the 2nd international consensus conference on laparoscopic liver resection. J Hepatobiliary Pancreat Sci 21:723–731
Soubrane O, Schwarz L, Cauchy F, Perotto LO, Brustia R, Bernard D, Scatton O (2015) A conceptual technique for laparoscopic right hepatectomy based on facts and oncologic principles: the caudal approach. Ann Surg 261:1226–1231
Ogiso S, Nomi T, Araki K, Conrad C, Hatano E, Uemoto S, Fuks D, Gayet B (2015) Laparoscopy-specific surgical concepts for hepatectomy based on the laparoscopic caudal view: a key to reboot surgeons’ minds. Ann Surg Oncol 22:327–333
Velayutham V, Fuks D, Nomi T, Kawaguchi Y, Gayet B (2016) 3D visualization reduces operating time when compared to high-definition 2D in laparoscopic liver resection: a case-matched study. Surg Endosc 30:147–153
Chaib E, Ribeiro MA Jr, Silva Fde S, Saad WA, Cecconello I (2007) Surgical approach for hepatic caudate lobectomy: review of 401 cases. J Am Coll Surg 204:118–127
Acknowledgments
We thank Dr. Mahendran Govindasamy for coordinating patient’s follow-up and maintaining the prospective database that formed the basis of this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Kenichiro Araki, David Fuks, Takeo Nomi, Satoshi Ogiso, Ruben R Lozano, Hiroyuki Kuwano, and Brice Gayet have no conflict of interest. Brice Gayet is consultant for Olympus.
Rights and permissions
About this article
Cite this article
Araki, K., Fuks, D., Nomi, T. et al. Feasibility of laparoscopic liver resection for caudate lobe: technical strategy and comparative analysis with anteroinferior and posterosuperior segments. Surg Endosc 30, 4300–4306 (2016). https://doi.org/10.1007/s00464-016-4747-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-4747-7