Abstract
Background
Therapeutic chances for metastatic melanoma have consistently changed over the last years with the advent of antibodies targeting the programmed cell death protein-1 (PD-1). Onset of immune-related adverse events (irAEs) during treatment can be a source of concern, and the association with survival outcome is yet to be defined.
Patients and methods
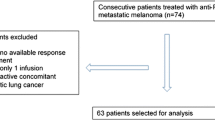
Data of consecutive patients treated with anti-PD1 (nivolumab or pembrolizumab) for metastatic melanoma between July 2013 and January 2018 were retrospectively reviewed. Baseline factors, together with onset of irAEs and vitiligo during treatment, were evaluated to identify predictors of progression-free (PFS) and overall (OS) survival. PFS and OS were assessed using Kaplan–Meier and Cox models.
Results
Overall, 173 patients were included in the present analysis, and 102 patients (59%) experienced irAEs. Disease control rate was 51%. Median (interquartile range) PFS and OS were 4.9 (2.6–13.3) and 8.6 (3.5–18.3) months, respectively. At multivariate analysis, irAEs occurrence was independently associated with improved PFS [HR 0.47 (95% CI 0.26, 0.86); p = 0.016], and correlated with better OS [HR 0.39 (95% CI 0.18, 0.81); p = 0.007]. Among various irAEs, the occurrence of vitiligo was associated with a trend toward a non-significant improved OS in comparison with other irAEs (p = 0.061). Median OS was undefined for patients experiencing vitiligo vs. 21.9 months for patients with other irAEs vs. 9.7 months for patients who had no irAEs (p = 0.003).
Conclusions
Our study underlines the association between irAEs and survival outcomes from anti-PD1 therapy. Careful management of treatment-related toxicity can lead to achieve maximum clinical benefit from this therapy.





Similar content being viewed by others
References
Boasberg PD, Hoon DS, Piro LD et al (2006) Enhanced survival associated with vitiligo expression during maintenance biotherapy for metastatic melanoma. J Invest Dermatol 126:2658–2663
Boudewijns S, Westdorp H, Koornstra RH et al (2016) Immune-related adverse events of dendritic cell vaccination correlate with immunologic and clinical outcome in stage III and IV melanoma patients. J Immunother 39:241–248
Bouwhuis MG, Ten Hagen TL, Suciu S, Eggermont AM (2011) Autoimmunity and treatment outcome in melanoma. Curr Opin Oncol 23:170–176
Brahmer JR, Lacchetti C, Schneider BJ et al (2018) Management of immune-related adverse events in patients treated with immune checkpoint inhibitor therapy: American Society of Clinical Oncology Clinical Practice Guideline. J Clin Oncol 36:1714–1768
Downey SG, Klapper JA, Smith FO et al (2007) Prognostic factors related to clinical response in patients with metastatic melanoma treated by CTL-associated antigen-4 blockade. Clin Cancer Res 12:6681–6688
Eggermont AMM, Christian UB, Blank MD et al (2018) Adjuvant pembrolizumab versus placebo in resected stage III melanoma. N Engl J Med 378:1789–1801
Feng Y, Roy A, Masson E et al (2013) Exposure-response relationships of the efficacy and safety of ipilimumab in patients with advanced melanoma. Clin Cancer Res 19:3977–3986
Freeman-Keller M, Kim Y, Cronin H (2016) Nivolumab in resected and unresectable metastatic melanoma: characteristics of immune-related adverse events and association with outcomes. Clin Cancer Res 22:886–894
Gogas H, Ioannovich J, Dafni U et al (2006) Prognostic significante of autoimmunity during treatment of melanoma with interferon. N Engl J Med 354:709–718
Heidelberger V, Goldwasser F, Kramkimel N et al (2017) Clinical parameters associated with anti-programmed death-1 (PD-1) inhibitors-induced tumor response in melanoma patients. Invest New Drugs 35:842–847
Hodi FS, O’Day SJ, McDermott DF et al (2010) Improved survival with ipilimumab in patients with metastatic melanoma. N Engl J Med 363:711–723
Hu Y, Smolkin ME, White EJ et al (2014) Inflammatory adverse events are associated with disease-free survival after vaccine therapy among patients with melanoma. Ann Surg Oncol 21:3978–3984
Hua C, Boussemart L, Mateus C (2016) Association of vitiligo with tumor response in patients with metastatic melanoma treated with pembrolizumab. JAMA Dermatol 152:45–51
Ku G, Yuan J, Page D et al (2010) Single-institution experience with ipilimumab in advanced melanoma patients in the compassionate use setting. Cancer 116:1767–1775
Larkin J, Chiarion-Sileni V, Gonzalez R et al (2015) Combined nivolumab and ipilimumab or monotherapy in untreated melanoma. N Engl J Med 373:23–34
Nakamura Y, Kitano S, Takahashi A et al (2016) Nivolumab for advanced melanoma: pretreatment prognostic factors and early outcome markers during therapy. Oncotarget 7:77404–77415
Nakamura Y, Tanaka R, Asami Y et al (2017) Correlation between vitiligo occurrence and clinical benefit in advanced melanoma patients treated with nivolumab: A multi-institutional retrospective study. J Dermatol 44:117–122
Nosrati A, Tsai KK, Goldinger SM et al (2017) Evaluation of clinicopathological factors in PD-1 response: derivation and validation of a prediction scale for response to PD-1 monotherapy. Br J Cancer 116:1141–1147
Ribas A, Puzanov I, Dummer R et al (2015) Pembrolizumab versus investigator-choice chemotherapy for ipilimumab-refractory melanoma (KEYNOTE-002): a randomised, controlled, phase 2 trial. Lancet Oncol 16:908–918
Robert C, Schachter J, Long GV et al (2015) Pembrolizumab versus Ipilimumab in Advanced Melanoma. N Engl J Med 372:2521–2532
Teulings HE, Limpens J, Jansen SN et al (2015) Vitiligo-like depigmentation in patients with stage III-IV melanoma receiving immunotherapy and its association with survival: a systematic review and meta-analysis. J Clin Oncol 33:773–781
Toi Y, Sugawara S, Kawashima Y et al (2018) Association of immune-related adverse events with clinical benefit in patients with advanced non-small-cell lung cancer treated with nivolumab. Oncologist 23:1358–1365
Topalian SL, Hodi FS, Brahmer JR et al (2012) Safety, activity and immune correlates of anti-PD-1 antibody in cancer. N Engl J Med 366:2443–2454
Wang DY, Salem JE, Cohen JV et al (2018) Fatal toxic effects associated with immune checkpoint inhibitors: a systematic review and meta-analysis. JAMA Oncol. https://doi.org/10.1001/jamaoncol.2018.3923
Weber JS, D’Angelo SP, Minor D et al (2015) Nivolumab versus chemotherapy in patients with advanced melanoma who progressed after anti-CTLA-4 treatment (CheckMate 037): a randomised, controlled, open-label, phase 3 trial. Lancet Oncol 16:375–384
Weber J, Mandala M, Del Vecchio M et al (2017a) Adjuvant nivolumab versus ipilimumab in resected stage III or IV melanoma. N Engl J Med 377:1824–1835
Weber JS, Hodi FS, Wolchok JD et al (2017b) Safety profile of nivolumab monotherapy: a pooled analysis of patients with advanced melanoma. J Clin Oncol 35:785–792
Weide B, Martens A, Hassel JC et al (2016) baseline biomarkers for outcome of melanoma patients treated with pembrolizumab. Clin Cancer Res 22:5487–5496
Funding
No fundings were received for the present investigation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Human rights and animal participants
This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Indini, A., Di Guardo, L., Cimminiello, C. et al. Immune-related adverse events correlate with improved survival in patients undergoing anti-PD1 immunotherapy for metastatic melanoma. J Cancer Res Clin Oncol 145, 511–521 (2019). https://doi.org/10.1007/s00432-018-2819-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-018-2819-x