Abstract
Purpose
Since herniotomy is one of the most frequent surgical procedures, the socioeconomical impact of guidelines for convalescence is substantial; at the same time, the introduction of mesh techniques as standard procedure has led to a marked decrease in recurrence rates. Therefore, a reappraisal of guidelines concerning convalescence is warranted.
Methods
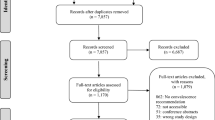
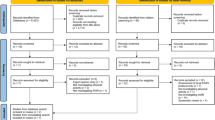
This study is a comprehensive review of the literature including all levels of evidence.
Results
If an inguinal hernia is repaired with an appropriate technique in a surgically and technically faultless contemporary procedure, it is fully stable immediately after surgery. Therefore, pain is the only rational limiting factor for physical activities after the intervention. If a patient wishes to go back to work or other activities early, there is no reason to not facilitate this via a generous prescription of analgesics. Even hard physical work can technically be resumed after complete healing of the skin wound, and prolonged sick leave is neither necessary nor beneficial. No interrelation between physical activity after herniotomy and recurrence rate has yet been demonstrated; a randomized controlled trial might finally clarify this question, but at a substantial effort.
Conclusions
The periods of inactivity practiced by patients and recommended by GPs are widely arbitrary and basically much too long, leading to unnecessary expenditures with an estimated order of magnitude of several hundred million € per year in Germany. To reduce this surplus, guidelines should be implemented by the surgical professional associations and communicated intensively towards GPs and patients.
Similar content being viewed by others
References
Holzheimer RG (2004) First results of Lichtenstein hernia repair with Ultrapro®-mesh as cost saving procedure—quality control combined with a modified quality of life questionnaire (SF-36) in a series of ambulatory operated patients. Eur J Med Res 9(6):323–327
Holzheimer RG (2005) Inguinal hernia: classification, diagnosis and treatment—classic, traumatic and Sportsman's hernia. Eur J Med Res 10(3):121–134
Kurzer M, Kark A, Hussain T (2007) Inguinal hernia repair. J Perioper Pract 17 (7):318–321, 323–316, 328–330
Schumpelick V, Stumpf M, Schwab R (2004) Leistenhernienchirurgie als ambulante und kurzzeitstationäre Chirurgie. Möglichkeiten und Grenzen. Chirurg 75(2):126–130. doi:10.1007/s00104-003-0777-5
Prieto-Díaz-Chávez E, Medina-Chávez JL, Anaya-Prado R (2009) A cost-effectiveness analysis of tension-free versus shouldice inguinal hernia repair: a randomized double-blind clinical trial. Hernia 13(3):233–238. doi:10.1007/s10029-008-0461-2
Gholghesaei M, Langeveld HR, Veldkamp R, Bonjer HJ (2005) Costs and quality of life after endoscopic repair of inguinal hernia vs open tension-free repair: a review. Surg Endosc 19(6):816–821. doi:10.1007/s00464-004-8949-z
Kuhry E, van Veen RN, Langeveld HR, Steyerberg EW, Jeekel J, Bonjer HJ (2007) Open or endoscopic total extraperitoneal inguinal hernia repair? A systematic review. Surg Endosc 21(2):161–166. doi:10.1007/s00464-006-0167-4
Subhas G, Bakston D, Gupta A, Jacobs MJ, Mittal VK, Silapaswan S (2010) Internal ring occlusion and floor support: a novel technique for inguinal hernia mesh repair. Am Surg 76(9):933–937
Simons MP, Aufenacker T, Bay-Nielsen M, Bouillot JL, Campanelli G, Conze J, de Lange D, Fortelny R, Heikkinen T, Kingsnorth A, Kukleta J, Morales-Conde S, Nordin P, Schumpelick V, Smedberg S, Smietanski M, Weber G, Miserez M (2009) European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia 13(4):343–403. doi:10.1007/s10029-009-0529-7
Bittner R, Arregui ME, Bisgaard T, Dudai M, Ferzli GS, Fitzgibbons RJ, Fortelny RH, Klinge U, Kockerling F, Kuhry E, Kukleta J, Lomanto D, Misra MC, Montgomery A, Morales-Conde S, Reinpold W, Rosenberg J, Sauerland S, Schug-Pass C, Singh K, Timoney M, Weyhe D, Chowbey P (2011) Guidelines for laparoscopic (TAPP) and endoscopic (TEP) treatment of inguinal hernia [International Endohernia Society (IEHS)]. Surg Endosc 25(9):2773–2843. doi:10.1007/s00464-011-1799-6
Aasvang EK, Gmaehle E, Hansen JB, Gmaehle B, Forman JL, Schwarz J, Bittner R, Kehlet H (2010) Predictive risk factors for persistent postherniotomy pain. Anesthesiology 112(4):957–969. doi:10.1097/ALN.0b013e3181d31ff8
Schmedt CG, Sauerland S, Bittner R (2005) Comparison of endoscopic procedures vs Lichtenstein and other open mesh techniques for inguinal hernia repair: a meta-analysis of randomized controlled trials. Surg Endosc 19(2):188–199. doi:10.1007/s00464-004-9126-0
Reuben B, Neumayer L (2006) Surgical management of inguinal hernia. Adv Surg 40:299–317
Alkhoury F, Martin JT, Contessa J, Zuckerman R, Nadzam G (2010) The impact of laparoscopy on the volume of open cases in general surgery training. J Surg Educ 67(5):316–319. doi:10.1016/j.jsurg.2010.08.001
Eklund AS, Montgomery AK, Rasmussen IC, Sandbue RP, Bergkvist LA, Rudberg CR (2009) Low recurrence rate after laparoscopic (TEP) and open (Lichtenstein) inguinal hernia repair: a randomized, multicenter trial with 5-year follow-up. Ann Surg 249(1):33–38. doi:10.1097/SLA.0b013e31819255d0
Nyhus LM (1989) The recurrent groin hernia: therapeutic solutions. World J Surg 13(5):541–544
Hendry PO, Paterson-Brown S, de Beaux A (2008) Work related aspects of inguinal hernia: a literature review. Surgeon 6(6):361–365
McIntosh A, Hutchinson A, Roberts A, Withers H (2000) Evidence-based management of groin hernia in primary care—a systematic review. Fam Pract 17(5):442–447
Bay-Nielsen M, Bisgaard T (2009) Rekonvalescens og sygemelding efter operation for lyskebrok. [Convalescence and sick leave following inguinal hernia repair]. Ugeskr Laeger 171(40):2899–2901
Lucht M (2008) Gesicherte Erkenntnisse zur Notwendigkeit einer körperlichen Schonung nach Leistenhernienoperation—Eine Evidenzbasierte Literaturstudie. Doctoral Thesis, Johann Wolfgang Goethe-Universität, Frankfurt/Main
Kavic MS (2005) Hernia repair: 2005. A reflection. Hernia 9(4):308–309. doi:10.1007/s10029-005-0001-2
McCormack K, Wake B, Perez J, Fraser C, Cook J, McIntosh E, Vale L, Grant A (2005) Laparoscopic surgery for inguinal hernia repair: systematic review of effectiveness and economic evaluation. Health Technol Assess 9(14):1–203, Ii–iv
Bourke JB, Taylor M (1978) The clinical and economic effects of early return to work after elective inguinal hernia repair. Br J Surg 65(10):728–731
Bourke JB, Lear PA, Taylor M (1981) Effect of early return to work after elective repair of inguinal hernia: clinical and financial consequences at one year and three years. Lancet 2(8247):623–625
Taylor EW, Dewar EP (1983) Early return to work after repair of a unilateral inguinal hernia. Br J Surg 70(10):599–600
Baker DM, Rider MA, Locker A, Fawcett AN (1993) How long do patients convalesce after inguinal herniorrhaphy? Current principles and practice. Ann R Coll Surg Engl 75(3):216
Baker DM, Rider MA, Fawcett AN (1994) When to return to work following a routine inguinal hernia repair: are doctors giving the correct advice? J R Coll Surg Edinb 39(1):31–33
Thorup J, Jørgensen T, Kjaergaard J, Billesbølle P (1994) Convalescence after inguinal herniorrhaphy. Scand J Gastroenterol 29(12):1150–1152
Bay-Nielsen M, Thomsen H, Andersen FH, Bendix JH, Sørensen OK, Skovgaard N, Kehlet H (2004) Convalescence after inguinal herniorrhaphy. Br J Surg 91(3):362–367. doi:10.1002/bjs.4437[doi]
Blodgett JB, Beattie EJ (1947) The effect of early postoperative rising on the recurrence rate of hernia. Surg Gynecol Obstet 84:716–718
Salcedo-Wasicek MC, Thirlby RC (1995) Postoperative course after inguinal herniorrhaphy. A case-controlled comparison of patients receiving workers' compensation vs patients with commercial insurance. Arch Surg 130(1):29–32
Chiofalo R, Holzinger F, Klaiber C (2001) Total endoskopische präperitoneale Netzplastik bei primären und Rezidivleistenhernien. Gibt es Unterschiede? Chirurg 72(12):1485–1491
Savarise MT, Simpson JP, Moore JM, Leis VM (2001) Improved functional outcome and more rapid return to normal activity following laparoscopic hernia repair. Surg Endosc 15(6):574–578. doi:10.1007/s004640080039[doi]
Pavlidis TE, Atmatzidis KS, Lazaridis CN, Papaziogas BT, Makris JG, Papaziogas TB (2002) Comparison between modern mesh and conventional non-mesh methods of inguinal hernia repair. Minerva Chir 57(1):7–12
Amid PK, Lichtenstein IL (1998) Long-term result and current status of the Lichtenstein open tension-free hernioplasty. Hernia 2:89–94
Quilici PJ, Greaney EM Jr, Quilici J, Anderson S (2000) Laparoscopic inguinal hernia repair: optimal technical variations and results in 1700 cases. Am Surg 66(9):848–852
Robertson GS, Burton PR, Haynes IG (1993) How long do patients convalescence after inguinal herniorrhaphy? Current principles and practice. Ann R Coll Surg Engl 75(1):30–33
Töns C, Muck-Töns A, Schumpelick V (1993) Leistenhernienchirurgie in Deutschland 1992: Eine Umfrage an 1656 deutschen Kliniken. Chirurg 64(8):635–641
Bachoo P, Duncan JL (1995) Prolonged convalescence following inguinal hernia repair: an unnecessary trend. Health Bull (Edinb) 53(4):209–212
Herzog U, Kocher T (1996) Leistenhernienchirurgie in der Schweiz 1994. Eine Umfrage an 142 Ausbildungskliniken in der Schweiz. Chirurg 67(9):921–926
van den Oever R, Debbaut B (1996) Kostenanalyse der Leistenhernienchirurgie bei ambulanter und stationärer Versorgung. Zentralbl Chir 121(10):836–840
Ciampolini J, Boyce DE, Shandall AA (1998) Adult hernia surgery in Wales revisited: impact of the guidelines of The Royal College of Surgeons of England. Ann R Coll Surg Engl 80(5):335–338
Kehlet H, Callesen T (1998) Recommendations for convalescence after hernia surgery. A questionnaire study. Ugeskr Laeger 160(7):1008–1009
Ismail W, Taylor SJ, Beddow E (2000) Advice on driving after groin hernia surgery in the United Kingdom: questionnaire survey. BMJ 321(7268):1056
Metzger J, Lutz N, Laidlaw I (2001) Guidelines for inguinal hernia repair in everyday practice. Ann R Coll Surg Engl 83(3):209–214
Rider MA, Baker DM, Locker A, Fawcett AN (1993) Return to work after inguinal hernia repair. Br J Surg 80(6):745–746
Callesen T, Klarskov B, Bech K, Kehlet H (1999) Short convalescence after inguinal herniorrhaphy with standardised recommendations: duration and reasons for delayed return to work. Eur J Surg 165(3):236–241. doi:10.1080/110241599750007108[doi]
Bay-Nielsen M, Perkins FM, Kehlet H (2001) Pain and functional impairment 1 year after inguinal herniorrhaphy: a nationwide questionnaire study. Ann Surg 233(1):1–7
Kumar S, Wilson RG, Nixon SJ, Macintyre IM (2002) Chronic pain after laparoscopic and open mesh repair of groin hernia. Br J Surg 89(11):1476–1479. doi:10.1046/j.1365-2168.2002.02260.x
Sajid MS, Leaver C, Baig MK, Sains P (2012) Systematic review and meta-analysis of the use of lightweight versus heavyweight mesh in open inguinal hernia repair. Br J Surg 99(1):29–37. doi:10.1002/bjs.7718
Kluivers KB, Hendriks JC, Mol BW, Bongers MY, Bremer GL, de Vet HC, Vierhout ME, Brolmann HA (2007) Quality of life and surgical outcome after total laparoscopic hysterectomy versus total abdominal hysterectomy for benign disease: a randomized, controlled trial. J Minim Invasive Gynecol 14(2):145–152. doi:10.1016/j.jmig.2006.08.009
Korolija D, Sauerland S, Wood-Dauphinee S, Abbou CC, Eypasch E, Caballero MG, Lumsden MA, Millat B, Monson JR, Nilsson G, Pointner R, Schwenk W, Shamiyeh A, Szold A, Targarona E, Ure B, Neugebauer E (2004) Evaluation of quality of life after laparoscopic surgery: evidence-based guidelines of the European Association for Endoscopic Surgery. Surg Endosc 18(6):879–897. doi:10.1007/s00464-003-9263-x
Le Blanc-Louvry I, Coquerel A, Koning E, Maillot C, Ducrotté P (2000) Operative stress response is reduced after laparoscopic compared to open cholecystectomy: the relationship with postoperative pain and ileus. Dig Dis Sci 45(9):1703–1713
McLauchlan GJ, Macintyre IM (1995) Return to work after laparoscopic cholecystectomy. Br J Surg 82(2):239–241
Ottesen M, Møller C, Kehlet H, Ottesen B (2001) Substantial variability in postoperative treatment, and convalescence recommendations following vaginal repair. A nationwide questionnaire study. Acta Obstet Gynecol Scand 80(11):1062–1068
Bokobza B (2002) Causes and mechanisms of recurrence after laparoscopic ventral hernia repair. In: Morales-Conde S (ed) Laparoscopic ventral hernia repair. Springer-Verlag, France, pp 451–461
Wara P, Bay-Nielsen M, Juul P, Bendix J, Kehlet H (2005) Prospective nationwide analysis of laparoscopic versus Lichtenstein repair of inguinal hernia. Br J Surg 92(10):1277–1281. doi:10.1002/bjs.5076[doi]
Bauer H, Fellmann E, Hermanek P, Hübner M, Jungnickel H, Kraas E, Ogasa J, Rückert K, Rümmelein D, Siefers H-F (2004) Leistenhernie. http://www.bqs-qualitaetsreport.de/2003/ergebnisse/leistungsbereiche/leistenhernie/. Accessed 28.12.2010
Ekman M, Johnell O, Lidgren L (2005) The economic cost of low back pain in Sweden in 2001. Acta Orthop 76(2):275–284
Hollinsky C, Göbl S (1999) Bursting strength evaluation after different types of mesh fixation in laparoscopic herniorrhaphy. Surg Endosc 13(10):958–961
Van’t Riet M, van Steenwijk De Vos PJ, Kleinrensink GJ, Steyerberg EW, Bonjer HJ (2002) Tensile strength of mesh fixation methods in laparoscopic incisional hernia repair. Surg Endosc 16(12):1713–1716. doi:10.1007/s00464-001-9202-7
Kumar A, Doran J, Batt ME, Nguyen-van-Tam JS, Beckingham IJ (2002) Results of inguinal canal repair in athletes with sports hernia. J R Coll Surg Edinb 47(3):561–565
Callesen T, Bech K, Nielsen R, Andersen J, Hesselfeldt P, Roikjaer O, Kehlet H (1998) Pain after groin hernia repair. Br J Surg 85(10):1412–1414. doi:10.1046/j.1365-2168.1998.00864.x[doi]
Gillion JF, Fagniez PL (1999) Chronic pain and cutaneous sensory changes after inguinal hernia repair: comparison between open and laparoscopic techniques. Hernia 3:75–80
Callesen T (2003) Inguinal hernia repair: anaesthesia, pain and convalescence. Dan Med Bull 50(3):203–218
Acknowledgments
The results were in part presented in the doctoral thesis of Mireille Untied (nee Lucht) at the University of Frankfurt in 2007 [20].
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Buhck, H., Untied, M. & Bechstein, W.O. Evidence-based assessment of the period of physical inactivity required after inguinal herniotomy. Langenbecks Arch Surg 397, 1209–1214 (2012). https://doi.org/10.1007/s00423-012-1008-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-012-1008-7