Abstract
Purpose
A study was conducted to investigate whether prolonged periods of very cold temperatures were associated with an increased risk of hospitalization for asthma.
Methods
Hospitalization admissions with a principal diagnosis of asthma were identified in New York State, USA, for the months November through April from 1991 to 2006. A cold spell was defined as three or more consecutive days where the daily mean of universal apparent temperature (UAT) within a week prior to admission was at the 10th percentile or less. The percentage change in asthma hospitalizations during and after a cold spell was compared to the average daily number of hospitalizations preceding the cold spell using time series analysis.
Results
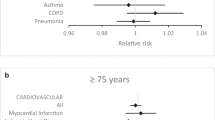
The average temperature during winter cold spells (December through March) was −15 °C, compared to −6 and −2 °C for cold spells in November and April, respectively. Cold spells during the winter months were associated with a mean decline of 4.9 % in asthma admissions statewide (95 % CI −7.8, −1.9 %). After a cold spell, no statistically significant changes were apparent during the winter months, but asthma hospitalizations increased after cold spells in the transitional months of November (mean = 9.6, 95 % CI 5.5, 13.9 %) and April (mean = 5.0, 95 % CI 1.2, 9.0 %).
Conclusions
The results suggest that during prolonged periods of severe cold asthmatics may adhere to medical guidelines and limit their exposure, thereby preventing exacerbations. They may be less likely to alter their behavior in the more moderate months of November and April.


Similar content being viewed by others
References
Estes TS (2011) Moving towards effective chronic illness management: asthma as an exemplar. Chron Respir Dis 8(3):163–170. doi:10.1177/1479972311412251
New York State Department of Health (NYSDOH) (2009) New York State Asthma Surveillance Summary Report. NYSDOH Public Health Information Group, Center for Community Health, Albany
Koenig JQ (1999) Air pollution and asthma. J Allergy Clin Immunol 104(4):717–722. doi:10.1016/S0091-6749(99)70280-0
Patel MM, Miller RL (2009) Air pollution and childhood asthma: recent advances and future directions. Curr Opin Pediatr 21(2):235–242. doi:10.1097/MOP.0b013e3283267726
Wong GW, Lai CK (2004) Outdoor air pollution and asthma. Curr Opin Pulm Med 10(1):62–66
Hales S, Lewis S, Slater T, Crane J, Pearce N (1998) Prevalence of adult asthma symptoms in relation to climate in New Zealand. Environ Health Perspect 106(9):607–610
Lin S, Luo M, Walker RJ, Liu X, Hwang SA, Chinery R (2009) Extreme high temperatures and hospital admissions for respiratory and cardiovascular diseases. Epidemiology 20(5):738–746. doi:10.1097/EDE.0b013e3181ad5522
Abe T, Tokuda Y, Ohde S, Ishimatsu S, Nakamura T, Birrer RB (2009) The relationship of short-term air pollution and weather to ED visits for asthma in Japan. Am J Emerg Med 27(2):153–159. doi:10.1016/j.ajem.2008.01.013
Gosai A, Salinger J, Dirks K (2009) Climate and respiratory disease in Auckland, New Zealand. Aust N Z J Public Health 33(3):521–526. doi:10.1111/j.1753-6405.2009.00447.x
Kim S, Kim Y, Lee MR, Kim J, Jung A, Park JS, Jang AS, Park SW, Uh ST, Choi JS, Kim YH, Buckley T, Park CS (2012) Winter season temperature drops and sulfur dioxide levels affect on exacerbation of refractory asthma in South Korea: a time-trend controlled case-crossover study using soonchunhyang asthma cohort data. J Asthma 49(7):679–687. doi:10.3109/02770903.2012.702839
Pönkä A (1991) Asthma and low level air pollution in Helsinki. Arch Environ Health 46(5):262–270
Steadman RG (1984) A universal scale of apparent temperature. J Climate Appl Meteorol 23(12):1674–1687
Kysely J, Pokorna L, Kyncl J, Kriz B (2009) Excess cardiovascular mortality associated with cold spells in the Czech Republic. BMC Public Health 9:19. doi:10.1186/1471-2458-9-19
Chinery R, Walker R (2009) Development of Exposure Characterization Regions for Priority Ambient Air Pollutants. Hum Ecol Risk Assess 15(5):876–889. doi:10.1080/10807030903152842
Environmental Protection Agency (2013) Ground Level Ozone. http://www.epa.gov/airquality/ozonepollution. Accessed 12-2-2013
Gu C (2002) Smoothing Spline ANOVA Models. Springer, New York
Guo Y, Jiang F, Peng L, Zhang J, Geng F, Xu J, Zhen C, Shen X, Tong S (2012) The association between cold spells and pediatric outpatient visits for asthma in Shanghai. China. PLoS One 7(7):e42232. doi:10.1371/journal.pone.0042232
Kaminsky DA, Bates JH, Irvin CG (2000) Effects of cool, dry air stimulation on peripheral lung mechanics in asthma. Am J Respir Crit Care Med 162(1):179–186
Koskela HO (2007) Cold air-provoked respiratory symptoms: the mechanisms and management. Int J Circumpolar Health 66(2):91–100. doi:10.3402/ijch.v66i2.18237
Li M, Li Q, Yang G, Kolosov VP, Perelman JM, Zhou XD (2011) Cold temperature induces mucin hypersecretion from normal human bronchial epithelial cells in vitro through a transient receptor potential melastatin 8 (TRPM8)-mediated mechanism. J Allergy Clin Immunol 128(3):626–634. doi:10.1016/j.jaci.2011.04.032
Butcher JD (2006) Exercise-induced asthma in the competitive cold weather athlete. Curr Sports Med Rep 5(6):284–288. doi:10.1097/01.CSMR.0000306431.39285.0b
Carlsen KH (2012) Sports in extreme conditions: the impact of exercise in cold temperatures on asthma and bronchial hyper-responsiveness in athletes. Br J Sports Med 46(11):796–799. doi:10.1136/bjsports-2012-091292
Uçok K, Dane S, Gökbel H, Akar S (2004) Prevalence of exercise-induced bronchospasm in long distance runners trained in cold weather. Lung 182(5):265–270. doi:10.1007/s00408-004-2503-6
Busse WW, Lemanske RF Jr (2007) Expert Panel Report 3: moving forward to improve asthma care. J Allergy Clin Immunol 120(5):1012–1014. doi:10.1016/j.jaci.2007.09.016
Acknowledgments
This work was supported in part by Grant # 5U01EH000396 from the National Center for Environmental Health, Centers for Disease Control and Prevention (CDCP), Atlanta, Georgia, USA. The content is solely the responsibility of the authors and does not necessarily represent the official view of CDCP.
Conflict of interest
The authors declare that they have no actual or potential conflicts of interest.
Ethical Standards
The study was approved for human subjects protection by the Institutional Review Board of the New York State Department of Health, Albany, NY, USA, and adheres to all current laws of the USA.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fitzgerald, E.F., Pantea, C. & Lin, S. Cold Spells and the Risk of Hospitalization for Asthma: New York, USA 1991–2006. Lung 192, 947–954 (2014). https://doi.org/10.1007/s00408-014-9645-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-014-9645-y