Abstract
Purpose
The association of complex dietary patterns with circulating selenoprotein P (SELENOP) levels in humans is unknown. In a general population sample, we aimed to identify a dietary pattern explaining inter-individual variation in circulating SELENOP concentrations and to study this pattern in relation to prevalent diabetes, metabolic syndrome (MetS), MRI-determined total volumes of visceral (VAT) and subcutaneous (SAT) abdominal adipose tissue, and liver signal intensity/fatty liver disease.
Methods
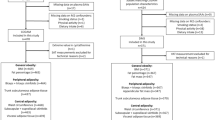
In this cross-sectional study, serum SELENOP levels were measured in 853 individuals. In a subsample of 553 participants, whole-body MRI was performed to assess body fat distribution and liver fat. Dietary intake was assessed by a self-administered food frequency questionnaire and the dietary pattern identified using reduced-rank regression (RRR). Multivariable linear and logistic regressions were used to investigate associations between dietary pattern score and metabolic traits.
Results
Characterized by high intake of fruit, vegetables and antioxidant beverages, the RRR-derived dietary pattern displayed inverse associations with VAT, SAT, MetS, and prevalent diabetes in multivariable-adjusted restricted cubic splines. Each unit increase in dietary pattern score was associated with 31% higher SELENOP levels, 12% lower VAT (95% CI: − 19%; − 5%), 13% (95% CI: − 20%; − 6%) lower SAT values and 46% (95% CI: 27%; 60%) and 53% (95% CI: 22%; 72%) lower odds of having MetS or diabetes, respectively. No meaningful relations were observed between the dietary pattern and liver traits.
Conclusions
Our observations propose diet-related regulation in SELENOP levels and that the identified dietary pattern is inversely related to VAT, SAT, MetS, and prevalent diabetes.




Similar content being viewed by others
References
Burk RF, Hill KE (2005) Selenoprotein P: an extracellular protein with unique physical characteristics and a role in selenium homeostasis. Annu Rev Nutr 25:215–235. https://doi.org/10.1146/annurev.nutr.24.012003.132120
Misu H, Takamura T, Takayama H, Hayashi H, Matsuzawa-Nagata N, Kurita S, Ishikura K, Ando H, Takeshita Y, Ota T, Sakurai M, Yamashita T, Mizukoshi E, Honda M, Miyamoto K, Kubota T, Kubota N, Kadowaki T, Kim HJ, Lee IK, Minokoshi Y, Saito Y, Takahashi K, Yamada Y, Takakura N, Kaneko S (2010) A liver-derived secretory protein, selenoprotein P, causes insulin resistance. Cell Metab 12(5):483–495. https://doi.org/10.1016/j.cmet.2010.09.015
di Giuseppe R, Koch M, Schlesinger S, Borggrefe J, Both M, Müller H, Kassubek J, Jacobs G, Nöthlings U, Lieb W (2017) Circulating selenoprotein P levels in relation to MRI-derived body fat volumes, liver fat content, and metabolic disorders. Obesity. https://doi.org/10.1002/oby.21841 (press)
Ko BJ, Kim SM, Park KH, Park HS, Mantzoros CS (2014) Levels of circulating selenoprotein P, fibroblast growth factor (FGF) 21 and FGF23 in relation to the metabolic syndrome in young children. Int J Obes (Lond) 38(12):1497–1502. https://doi.org/10.1038/ijo.2014.45
Choi HY, Hwang SY, Lee CH, Hong HC, Yang SJ, Yoo HJ, Seo JA, Kim SG, Kim NH, Baik SH, Choi DS, Choi KM (2013) Increased selenoprotein p levels in subjects with visceral obesity and nonalcoholic Fatty liver disease. Diabetes Metab J 37(1):63–71. https://doi.org/10.4093/dmj.2013.37.1.63
Persson-Moschos M, Alfthan G, Akesson B (1998) Plasma selenoprotein P levels of healthy males in different selenium status after oral supplementation with different forms of selenium. Eur J Clin Nutr 52(5):363–367
Hill KE, Xia Y, Akesson B, Boeglin ME, Burk RF (1996) Selenoprotein P concentration in plasma is an index of selenium status in selenium-deficient and selenium-supplemented Chinese subjects. J Nutr 126(1):138–145
Duffield AJ, Thomson CD, Hill KE, Williams S (1999) An estimation of selenium requirements for New Zealanders. Am J Clin Nutr 70(5):896–903
Outzen M, Tjonneland A, Larsen EH, Andersen KK, Christensen J, Overvad K, Olsen A (2015) The effect on selenium concentrations of a randomized intervention with fish and mussels in a population with relatively low habitual dietary selenium intake. Nutrients 7(1):608–624. https://doi.org/10.3390/nu7010608
Hu FB (2002) Dietary pattern analysis: a new direction in nutritional epidemiology. Curr Opin Lipidol 13(1):3–9
Hoffmann K, Schulze MB, Schienkiewitz A, Nothlings U, Boeing H (2004) Application of a new statistical method to derive dietary patterns in nutritional epidemiology. Am J Epidemiol 159(10):935–944
Nothlings U, Krawczak M (2012) PopGen. A population-based biobank with prospective follow-up of a control group. Bundesgesundheitsblatt Gesundheitsforschung Gesundheitsschutz 55(6–7):831–835. https://doi.org/10.1007/s00103-012-1487-2
Koch M, Borggrefe J, Barbaresko J, Groth G, Jacobs G, Siegert S, Lieb W, Muller MJ, Bosy-Westphal A, Heller M, Nothlings U (2014) Dietary patterns associated with magnetic resonance imaging-determined liver fat content in a general population study. Am J Clin Nutr 99(2):369–377. https://doi.org/10.3945/ajcn.113.070219
Nothlings U, Hoffmann K, Bergmann MM, Boeing H (2007) Fitting portion sizes in a self-administered food frequency questionnaire. J Nutr 137(12):2781–2786
Barbaresko J, Siegert S, Koch M, Aits I, Lieb W, Nikolaus S, Laudes M, Jacobs G, Nothlings U (2014) Comparison of two exploratory dietary patterns in association with the metabolic syndrome in a Northern German population. Br J Nutr 112(8):1364–1372. https://doi.org/10.1017/S0007114514002098
Kroger J, Ferrari P, Jenab M, Bamia C, Touvier M, Bueno-de-Mesquita HB, Fahey MT, Benetou V, Schulz M, Wirfalt E, Boeing H, Hoffmann K, Schulze MB, Orfanos P, Oikonomou E, Huybrechts I, Rohrmann S, Pischon T, Manjer J, Agren A, Navarro C, Jakszyn P, Boutron-Ruault MC, Niravong M, Khaw KT, Crowe F, Ocke MC, van der Schouw YT, Mattiello A, Bellegotti M, Engeset D, Hjartaker A, Egeberg R, Overvad K, Riboli E, Bingham S, Slimani N (2009) Specific food group combinations explaining the variation in intakes of nutrients and other important food components in the European Prospective Investigation into Cancer and Nutrition: an application of the reduced rank regression method. Eur J Clin Nutr 63(Suppl 4):S263–S274. https://doi.org/10.1038/ejcn.2009.85
Colditz GA, Willett WC (1991) Epidemiologic approaches to the study of diet and cancer. In: AlfSlater RB, Kritchevsky D, AlfSlater RB, Kritchevsky D (eds) Cancer and nutrition se epidemiologic approaches to the study of diet and cancer, 1st edn. Springer, New York, pp 58–60
Karita K, Sasaki S, Ishihara J, Tsugane S (2003) Validity of a self-administered food frequency questionnaire used in the 5-year follow-up survey of the JPHC Study to assess selenium intake: comparison with dietary records and blood levels. J Epidemiol 13(1 Suppl):S92-97
Hurst R, Armah CN, Dainty JR, Hart DJ, Teucher B, Goldson AJ, Broadley MR, Motley AK, Fairweather-Tait SJ (2010) Establishing optimal selenium status: results of a randomized, double-blind, placebo-controlled trial. Am J Clin Nutr 91(4):923–931. https://doi.org/10.3945/ajcn.2009.28169
Stoffaneller R, Morse NL (2015) A review of dietary selenium intake and selenium status in Europe and the Middle East. Nutrients 7(3):1494–1537. https://doi.org/10.3390/nu7031494
Ainsworth BE, Haskell WL, Herrmann SD, Meckes N, Bassett DR Jr, Tudor-Locke C, Greer JL, Vezina J, Whitt-Glover MC, Leon AS (2011) Compendium of physical activities: a second update of codes and MET values. Med Sci Sports Exerc 43(8):1575–1581. https://doi.org/10.1249/MSS.0b013e31821ece12
Alberti KG, Eckel RH, Grundy SM, Zimmet PZ, Cleeman JI, Donato KA, Fruchart JC, James WP, Loria CM, Smith SC Jr (2009) Harmonizing the metabolic syndrome: a joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation 120(16):1640–1645. https://doi.org/10.1161/CIRCULATIONAHA.109.192644
Fischer K, Moewes D, Koch M, Muller HP, Jacobs G, Kassubek J, Lieb W, Nothlings U (2015) MRI-determined total volumes of visceral and subcutaneous abdominal and trunk adipose tissue are differentially and sex-dependently associated with patterns of estimated usual nutrient intake in a northern German population. Am J Clin Nutr 101(4):794–807. https://doi.org/10.3945/ajcn.114.101626
Muller HP, Raudies F, Unrath A, Neumann H, Ludolph AC, Kassubek J (2011) Quantification of human body fat tissue percentage by MRI. NMR Biomed 24(1):17–24. https://doi.org/10.1002/nbm.1549
Szczepaniak LS, Nurenberg P, Leonard D, Browning JD, Reingold JS, Grundy S, Hobbs HH, Dobbins RL (2005) Magnetic resonance spectroscopy to measure hepatic triglyceride content: prevalence of hepatic steatosis in the general population. Am J Physiol Endocrinol Metab 288(2):E462-468. https://doi.org/10.1152/ajpendo.00064.2004
Willett WC, Howe GR, Kushi LH (1997) Adjustment for total energy intake in epidemiologic studies. Am J Clin Nutr 65 (4 Suppl):1220S–1228S. (Discussion 1229S-1231S)
Hu FB, Rimm E, Smith-Warner SA, Feskanich D, Stampfer MJ, Ascherio A, Sampson L, Willett WC (1999) Reproducibility and validity of dietary patterns assessed with a food-frequency questionnaire. Am J Clin Nutr 69(2):243–249
McNaughton SA, Mishra GD, Brunner EJ (2008) Dietary patterns, insulin resistance, and incidence of type 2 diabetes in the Whitehall II Study. Diabetes Care 31(7):1343–1348. https://doi.org/10.2337/dc07-1946
Desquilbet L, Mariotti F (2010) Dose-response analyses using restricted cubic spline functions in public health research. Stat Med 29(9):1037–1057. https://doi.org/10.1002/sim.3841
Xia Y, Hill KE, Byrne DW, Xu J, Burk RF (2005) Effectiveness of selenium supplements in a low-selenium area of China. Am J Clin Nutr 81(4):829–834
Meplan C, Crosley LK, Nicol F, Beckett GJ, Howie AF, Hill KE, Horgan G, Mathers JC, Arthur JR, Hesketh JE (2007) Genetic polymorphisms in the human selenoprotein P gene determine the response of selenoprotein markers to selenium supplementation in a gender-specific manner (the SELGEN study). FASEB J 21(12):3063–3074. https://doi.org/10.1096/fj.07-8166com
Hagmar L, Persson-Moschos M, Akesson B, Schutz A (1998) Plasma levels of selenium, selenoprotein P and glutathione peroxidase and their correlations to fish intake and serum levels of thyrotropin and thyroid hormones: a study on Latvian fish consumers. Eur J Clin Nutr 52(11):796–800
Huang W, Akesson B, Svensson BG, Schutz A, Burk RF, Skerfving S (1995) Selenoprotein P and glutathione peroxidase (EC 1.11.1.9) in plasma as indices of selenium status in relation to the intake of fish. Br J Nutr 73(3):455–461
Rasmussen LB, Hollenbach B, Laurberg P, Carle A, Hog A, Jorgensen T, Vejbjerg P, Ovesen L, Schomburg L (2009) Serum selenium and selenoprotein P status in adult Danes—8-year followup. J Trace Elem Med Biol 23(4):265–271. https://doi.org/10.1016/j.jtemb.2009.03.009
Combs GF Jr (2015) Biomarkers of selenium status. Nutrients 7(4):2209–2236. https://doi.org/10.3390/nu7042209
Daniels LA (1996) Selenium metabolism and bioavailability. Biol Trace Elem Res 54(3):185–199. https://doi.org/10.1007/BF02784430
Sobiecki JG (2017) Vegetarianism and colorectal cancer risk in a low-selenium environment: effect modification by selenium status? A possible factor contributing to the null results in British vegetarians. Eur J Nutr 56(5):1819–1832. https://doi.org/10.1007/s00394-016-1364-0
Renko K, Martitz J, Hybsier S, Heynisch B, Voss L, Everley RA, Gygi SP, Stoedter M, Wisniewska M, Kohrle J, Gladyshev VN, Schomburg L (2017) Aminoglycoside-driven biosynthesis of selenium-deficient Selenoprotein P. Sci Rep 7(1):4391. https://doi.org/10.1038/s41598-017-04586-9
Renko K, Hofmann PJ, Stoedter M, Hollenbach B, Behrends T, Kohrle J, Schweizer U, Schomburg L (2009) Down-regulation of the hepatic selenoprotein biosynthesis machinery impairs selenium metabolism during the acute phase response in mice. FASEB J 23(6):1758–1765. https://doi.org/10.1096/fj.08-119370
Hesse-Bahr K, Dreher I, Kohrle J (2000) The influence of the cytokines Il-1beta and INFgamma on the expression of selenoproteins in the human hepatocarcinoma cell line HepG2. Biofactors 11(1–2):83–85
Haug A, Graham RD, Christophersen OA, Lyons GH (2007) How to use the world’s scarce selenium resources efficiently to increase the selenium concentration in food. Microb Ecol Health Dis 19(4):209–228. https://doi.org/10.1080/08910600701698986
Ogawa-Wong AN, Berry MJ, Seale LA (2016) Selenium and metabolic disorders: an emphasis on type 2. Diabetes Risk Nutr 8(2):80. https://doi.org/10.3390/nu8020080
Joseph J (2013) Selenium and cardiometabolic health: inconclusive yet intriguing evidence. Am J Med Sci 346(3):216–220. https://doi.org/10.1097/MAJ.0b013e3182638716
Stranges S, Marshall JR, Natarajan R, Donahue RP, Trevisan M, Combs GF, Cappuccio FP, Ceriello A, Reid ME (2007) Effects of long-term selenium supplementation on the incidence of type 2 diabetes: a randomized trial. Ann Intern Med 147(4):217–223
Lippman SM, Klein EA, Goodman PJ, Lucia MS, Thompson IM, Ford LG, Parnes HL, Minasian LM, Gaziano JM, Hartline JA, Parsons JK, Bearden JD, 3rd, Crawford ED, Goodman GE, Claudio J, Winquist E, Cook ED, Karp DD, Walther P, Lieber MM, Kristal AR, Darke AK, Arnold KB, Ganz PA, Santella RM, Albanes D, Taylor PR, Probstfield JL, Jagpal TJ, Crowley JJ, Meyskens FL Jr, Baker LH, Coltman CA, Jr (2009) Effect of selenium and vitamin E on risk of prostate cancer and other cancers: the Selenium and Vitamin E Cancer Prevention Trial (SELECT). JAMA 301(1):39–51. https://doi.org/10.1001/jama.2008.864
Stranges S, Navas-Acien A, Rayman MP, Guallar E (2010) Selenium status and cardiometabolic health: state of the evidence. Nutr Metab Cardiovasc Dis 20(10):754–760. https://doi.org/10.1016/j.numecd.2010.10.001
Reszka E, Jablonska E, Gromadzinska J, Wasowicz W (2012) Relevance of selenoprotein transcripts for selenium status in humans. Genes Nutr 7(2):127–137. https://doi.org/10.1007/s12263-011-0246-6
Carnauba RA, Chaves DF, Baptistella AB, Paschoal V, Naves A, Buehler AM (2016) Association between high consumption of phytochemical-rich foods and anthropometric measures: a systematic review. Int J Food Sci Nutr 1–9. https://doi.org/10.1080/09637486.2016.1229761
Rodriguez-Monforte M, Sanchez E, Barrio F, Costa B, Flores-Mateo G (2016) Metabolic syndrome and dietary patterns: a systematic review and meta-analysis of observational studies. Eur J Nutr. https://doi.org/10.1007/s00394-016-1305-y
Gamboa-Gomez CI, Rocha-Guzman NE, Gallegos-Infante JA, Moreno-Jimenez MR, Vazquez-Cabral BD, Gonzalez-Laredo RF (2015) Plants with potential use on obesity and its complications. EXCLI J 14:809–831. https://doi.org/10.17179/excli2015-186
Groenwold RH, Klungel OH, Altman DG, van der Graaf Y, Hoes AW, Moons KG (2013) Adjustment for continuous confounders: an example of how to prevent residual confounding. CMAJ 185(5):401–406. https://doi.org/10.1503/cmaj.120592
Altinova AE, Iyidir OT, Ozkan C, Ors D, Ozturk M, Gulbahar O, Bozkurt N, Toruner FB, Akturk M, Cakir N, Arslan M (2015) Selenoprotein P is not elevated in gestational diabetes mellitus. Gynecol Endocrinol 31(11):874–876. https://doi.org/10.3109/09513590.2015.1103220
Chen M, Liu B, Wilkinson D, Hutchison AT, Thompson CH, Wittert GA, Heilbronn LK (2017) Selenoprotein P is elevated in individuals with obesity, but is not independently associated with insulin resistance. Obes Res Clin Pract 11(2):227–232. https://doi.org/10.1016/j.orcp.2016.07.004
Acknowledgements
R.d.G. is supported by the Deutsche Forschungsgemeinschaft Excellence Cluster “Inflammation at Interfaces” (Grant EXC306/2). Koch M. is recipient of a Postdoctoral Research Fellowship from the German Research Foundation (DFG, Deutsche Forschungsgemeinschaft). The PopGen 2.0 network is supported by the German Federal Ministry of Education and Research (Grant 01EY1103).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
di Giuseppe, R., Plachta-Danielzik, S., Koch, M. et al. Dietary pattern associated with selenoprotein P and MRI-derived body fat volumes, liver signal intensity, and metabolic disorders. Eur J Nutr 58, 1067–1079 (2019). https://doi.org/10.1007/s00394-018-1624-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-018-1624-2