Abstract
Purpose
To compare the degree of necrotizing enterocolitis (NEC)-like damage under different stress conditions in neonatal mice.
Methods
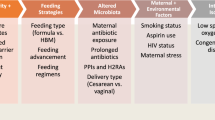
5-day-old C57BL/6 mice were assigned to: (A) breastfed and no stress factors; (B) breastfed+maternal separation (3 h daily); (C) breastfed+hypoxia+lipopolysaccharide (LPS–4 mg/kg/day); (D) hyperosmolar formula+hypoxia+LPS. Mice were killed at 9 days of life. Ileum and colon were stained for hematoxylin/eosin and blindly assessed. A scoring ≥2 was considered NEC. Data were compared using one-way ANOVA and reported as median (range).
Results
Ileum—Mucosal injury was mild in group B (0.0–1). Hypoxia+LPS induced greater injury in group C (1.6, 1–2.5; p < 0.0001 to B) and D (2, 0.5–3.5; p < 0.0001 to B). There were no differences between group C and D (p = n.s.). There were no cases of NEC in group A or B, whereas NEC was present in 36 % group C and 68 % group D mice. Colon—a similar degree of mucosal injury was observed among group B (2, 1–3), C (1.7, 0–3) and D (1.5, 1–3; p = n.s.). NEC was present in 75 % of group B, 50 % of group C and 86 % of group D.
Conclusion
These models establish a spectrum of intestinal injury and are useful to investigate the variability of neonatal intestinal diseases, such as NEC.


Similar content being viewed by others
References
Fitzgibbons SC, Ching Y, Yu D et al (2009) Mortality of necrotizing enterocolitis expressed by birth weight categories. J Pediatr Surg 44:1072–1075
Neu J, Walker WA (2011) Necrotizing enterocolitis. N Engl J Med 364:255–264
Barlow B, Santulli TV, Heird WC et al (1974) An experimental study of acute neonatal enterocolitis—the importance of breast milk. J Pediatr Surg 9:587–595
Grishin AV, Wang J, Potoka DA et al (2006) Lipopolysaccharide induces cyclooxygenase-2 in intestinal epithelium via a non canonical p 38 MAPK pathway. J Immunol 176:580–588
Zamora R, Bryan NS, Boyle P et al (2005) Nitrosative stress in an animal model of necrotizing enterocolitis. Free Radic Biol Med 39:1428–1437
Zani A, Cordischi L, Cananzi M et al (2008) Assessment of a neonatal rat model of necrotizing enterocolitis. Eur J Pediatr Surg 18:423–426
Zani A, Eaton S, Leon FF et al (2008) Captopril reduces the severity of bowel damage in a neonatal rat model of necrotizing enterocolitis. J Pediatr Surg 43:308–314
Jilling T, Simon D, Lu J et al (2006) The roles of bacteria and TLR4 in rat and murine models of necrotizing enterocolitis. J Immunol 177:3273–3282
Cetin S, Leaphart CL, Li J et al (2007) Nitric oxide inhibits enterocyte migration through activation of RhoA-GTPase in a SHP-2-dependent manner. Am J Physiol Gastrointest Liver Physiol 292:G1347–G1358
Leaphart CL, Qureshi F, Cetin S et al (2007) Interferon-gamma inhibits intestinal restitution by preventing gap junction communication between enterocytes. Gastroenterology 132:2395–2411
Baregamian N, Rychahou PG, Hawkins HK et al (2007) Phosphatidylinositol 3-kinase pathway regulates hypoxia-inducible factor-1 to protect from intestinal injury during necrotizing enterocolitis. Surgery 142:295–302
Halpern MD, Khailova L, Molla-Hosseini D et al (2008) Decreased development of necrotizing enterocolitis in IL-18-deficient mice. Am J Physiol Gastrointest Liver Physiol 294:G20–G26
El-Assal ON, Paddock H, Marquez A et al (2008) Heparin-binding epidermal growth factor-like growth factor gene disruption is associated with delayed intestinal restitution, impaired angiogenesis, and poor survival after intestinal ischemia in mice. J Pediatr Surg 43:1182–1190
Spencer-Booth Y, Hinde RA (1966) The effects of separating rhesus monkey infants from their mothers for 6 days. J Child Psychol Psychiatry 7:179–197
Ackerman SH, Hofer MA, Weiner H (1978) Early maternal separation increases gastric ulcer risk in rats by producing a latent thermoregulatory disturbance. Science 201:373–376
Bailey MT, Coe CL (1999) Maternal separation disrupts the integrity of the intestinal microflora in infant rhesus monkeys. Dev Psychobiol 35:146–155
Söderholm JD, Yates DA, Gareau MG et al (2002) Neonatal maternal separation predisposes adult rats to colonic barrier dysfunction in response to mild stress. Am J Physiol Gastrointest Liver Physiol 283:G1257–G1263
Barreau F, Ferrier L, Fioramonti J et al (2004) Neonatal maternal deprivation triggers long term alterations in colonic epithelial barrier and mucosal immunity in rats. Gut 53:501–506
Gareau MG, Jury J, Yang PC et al (2006) Neonatal maternal separation causes colonic dysfunction in rat pups including impaired host resistance. Pediatr Res 59:83–88
Li B, Lee C, Zani A et al (2014) Early maternal separation induces alterations of colonic epithelial permeability and morphology. Pediatr Surg Int 30:1217–1222
Barreau F, Ferrier L, Fioramonti J et al (2007) New insights in the etiology and pathophysiology of irritable bowel syndrome: contribution of neonatal stress models. Pediatr Res 62:240–245
Lennon EM, Maharshak N, Elloumi H et al (2013) Early life stress triggers persistent colonic barrier dysfunction and exacerbates colitis in adult IL-10−/− mice. Inflamm Bowel Dis 19:712–719
Radulescu A, Zhang HY, Yu X et al (2010) Heparin-binding epidermal growth factor-like growth factor overexpression in transgenic mice increases resistance to necrotizing enterocolitis. J Pediatr Surg 45:1933–1939
Tian R, Liu SX, Williams C et al (2010) Characterization of a necrotizing enterocolitis model in newborn mice. Int J Clin Exp Med 3:293–302
Mortell A, Montedonico S, Puri P (2006) Animal models in pediatric surgery. Pediatr Surg Int 22:111–128
Moussaoui N, Braniste V, Ait-Belgnaoui A et al (2014) Changes in intestinal glucocorticoid sensitivity in early life shape the risk of epithelial barrier defect in maternal-deprived rats. PLoS One 9:e88382
Sodhi C, Richardson W, Gribar S et al (2008) The development of animal models for the study of necrotizing enterocolitis. Dis Model Mech 1:94–98
Lucas A, Cole TJ (1990) Breast milk and neonatal necrotising enterocolitis. Lancet 336:1519–1523
Quigley MA, Henderson G, Anthony MY et al (2007) Formula milk versus donor breast milk for feeding preterm or low birth weight infants. Cochrane Database Syst Rev 4:CD002971
Quigley M, McGuire W (2014) Formula versus donor breast milk for feeding preterm or low birth weight infants. Cochrane Database Syst Rev 4:CD002971
Dvorak B, Halpern MD, Holubec H et al (2003) Maternal milk reduces severity of necrotizing enterocolitis and increases intestinal IL-10 in a neonatal rat model. Pediatr Res 53:426–433
Reisner SH, Garty B (1977) Necrotising enterocolitis despite breast feeding. Lancet 2:507
Moriartey RR, Finer NN, Cox SF et al (1979) Necrotizing enterocolitis and human milk. J Pediatr 94:295–296
Section on Breastfeeding (2012) Breastfeeding and the use of human milk. Pediatrics 129:e827–e841
Palmer SR, Thomas SJ, Cooke RW et al (1987) Birthweight-specific risk factors for necrotising enterocolitis. J Epidemiol Community Health 41:210–214
Guven A, Gundogdu G, Uysal B et al (2009) Hyperbaric oxygen therapy reduces the severity of necrotizing enterocolitis in a neonatal rat model. J Pediatr Surg 44:534–540
Patel RM, Denning PW (2015) Intestinal microbiota and its relationship with necrotizing enterocolitis. Pediatr Res 78:232–238
Barlow B, Santulli TV (1975) Importance of multiple episodes of hypoxia or cold stress on the development of enterocolitis in an animal model. Surgery 77:687–690
Caplan MS, Hedlund E, Adler L et al (1994) Role of asphyxia and feeding in a neonatal rat model of necrotizing enterocolitis. Pediatr Pathol 14:1017–1028
Hunter CJ, Singamsetty VK, Chokshi NK et al (2008) Enterobacter sakazakii enhances epithelial cell injury by inducing apoptosis in a rat model of necrotizing enterocolitis. J Infect Dis 198:586–593
Acknowledgments
This work was supported by the endowment of the Robert M Filler Chair of Surgery, The Hospital for Sick Children.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zani, A., Zani-Ruttenstock, E., Peyvandi, F. et al. A spectrum of intestinal injury models in neonatal mice. Pediatr Surg Int 32, 65–70 (2016). https://doi.org/10.1007/s00383-015-3813-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-015-3813-x