Abstract
Background
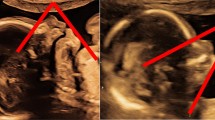
This study aimed to evaluate postnatal outcome of fetuses affected by nonprogressive, isolated, mild (≥10 and ≤12 mm) borderline ventriculomegaly (BVM).
Methods
We studied 25 consecutive fetuses with BMV and evaluated patients' characteristic, ultrasonographic findings, and the neurodevelopmental outcome at age ≥24 months.
Results
The mean gestational age at diagnosis was 23.84 ± 5.02 weeks (min–max; 17–34 weeks). In 16 cases, BVM was bilateral (16/25, 64 %), 4 left sided (4/25, 16 %), and 5 right sided (5/25, 20 %). Fourteen cases were males (14/25, 56 %), and 11 cases were females (11/25, 44 %). In two cases, ventriculomegaly was regressed 4 weeks after the initial diagnosis (2/25, 8 %), and in the remaining cases, ventriculomegaly persisted between initial measurement and 12 mm. The mean age of the infant at the time of the neurodevelopmental evaluation was 45.9 months (24–77 months). The neurodevelopmental outcome at the mean age of 45.9 months was completely normal in 16 infants (16/25, 64 %). The remaining nine infants (9/25, 36 %) had mild degree of neuromotor developmental delay.
Conclusion
Prenatal counseling for isolated, nonprogressive, mild BVM should be mainly reassurance since it is not associated with severe neurodevelopmental delay. However, parents should be educated about the developmental milestone of children to observe and detect mild neurodevelopmental delay which can be associated with mild BVM.


Similar content being viewed by others
References
Bromley B, Frigoletto FD Jr, Benacerraf BR (1991) Mild fetal lateral cerebral ventriculomegaly: clinical course and outcome. Am J Obstet Gynecol 164:863–886
Cardoza JD, Goldstein RB, Filly RA (1988) Exclusion of fetal ventriculomegaly with a single measurement: the width of the lateral ventricular atrium. Radiology 169:711–714
Ertem IO, Atay G, Dogan DG, Bayhan A, Bingoler BE, Gok CG, Ozbas S, Haznedaroglu D, Isikli S (2007) Mothers' knowledge of young child development in a developing country. Child Care Health Dev 33:728–737
Falip C, Blanc N, Maes E, Zaccaria I, Oury JF, Sebag G, Garel C (2007) Postnatal clinical and imaging follow-up of infants with prenatal isolated mild ventriculomegaly: a series of 101 cases. Pediatr Radiol 37:981–989
Gaglioti P, Danelon D, Bontempo S, Mombrò M, Cardaropoli S, Todros T (2005) Fetal cerebral ventriculomegaly: outcome in 176 cases. Ultrasound Obstet Gynecol 25:372–3777
Garel C, Luton D, Oury JF, Gressens P (2003) Ventricular dilatations. Childs Nerv Syst 19:517–523
Gilmore JH, van Tol J, Kliewer MA, Silva SG, Cohen SB, Hertzberg BS, Chescheir NC (1998) Mild ventriculomegaly detected in utero with ultrasound: clinical associations and implications for schizophrenia. Schizophr Res 33:133–140
Gómez-Arriaga P, Herraiz I, Puente JM, Zamora-Crespo B, Núñez-Enamorado N, Galindo A (2012) Mid-term neurodevelopmental outcome in isolated mild ventriculomegaly diagnosed in fetal life. Fetal Diagn Ther 31:12–18
Greco P, Vimercati A, De Cosmo L, Laforgia N, Mautone A, Selvaggi L (2001) Mild ventriculomegaly as a counselling challenge. Fetal Diagn Ther 16:398–401
Lipitz S, Yagel S, Malinger G, Meizner I, Zalel Y, Achiron R (1998) Outcome of fetuses with isolated borderline unilateral ventriculomegaly diagnosed at mid-gestation. Ultrasound Obstet Gynecol 12:23–26
Melchiorre K, Bhide A, Gika AD, Pilu G, Papageorghiou AT (2009) Counseling in isolated mild fetal ventriculomegaly. Ultrasound Obstet Gynecol 34:212–224
Melchiorre K, Liberati M, Celentano C, Domizio S, Puglielli C, Buoni S, Strambi M, Zannolli R (2009) Neurological outcome following isolated 10–12 mm fetal ventriculomegaly. Arch Dis Child Fetal Neonatal Ed 94:F311–F312
Parazzini C, Righini A, Doneda C, Arrigoni F, Rustico M, Lanna M, Triulzi F (2012) Is fetal magnetic resonance imaging indicated when ultrasound isolated mild ventriculomegaly is present in pregnancies with no risk factors? Prenat Diagn 32:752–757
Picone O, Simon I, Benachi A, Brunelle F, Sonigo P (2008) Comparison between ultrasound and magnetic resonance imaging in assessment of fetal cytomegalovirus infection. Prenat Diagn 28:753–758
Pilu G, Hobbins JC (2002) Sonography of fetal cerebrospinal anomalies. Prenat Diagn 22:321–330
Piven J, Arndt S, Bailey J, Havercamp S, Andreasen NC, Palmer P (1995) An MRI study of brain size in autism. Am J Psychiatry 152:1145–1149
Salomon LJ, Ouahba J, Delezoide AL, Vuillard E, Oury JF, Sebag G, Garel C (2006) Third-trimester fetal MRI in isolated 10- to 12-mm ventriculomegaly: is it worth it? BJOG 113:942–947
Salomon LJ, Garel C (2007) Magnetic resonance imaging examination of the fetal brain. Ultrasound Obstet Gynecol 30:1019–1032
Signorelli M, Tiberti A, Valseriati D, Molin E, Cerri V, Groli C, Bianchi UA (2004) Width of the fetal lateral ventricular atrium between 10 and 12 mm: a simple variation of the norm? Ultrasound Obstet Gynecol 23:14–18
Tatlı B, Özer I, Ekici B, Kalelioğlu I, Has R, Eraslan E, Yüksel A (2012) Neurodevelopmental outcome of 31 patients with borderline fetal ventriculomegaly. Clin Neurol Neurosurg 114:969–971
Vergani P, Locatelli A, Strobelt N, Cavallone M, Ceruti P, Paterlini G, Ghidini A (1998) Clinical outcome of mild fetal ventriculomegaly. Am J Obstet Gynecol 178:218–222
Wang KC, Lee JY, Kim SK, Phi JH, Cho BK (2011) Fetal ventriculomegaly: postnatal management. Childs Nerv Syst 27:1571–1573
World Health Organization (1980) International classification of impairments, disabilities and handicaps: manual of classification relating to the consequences of disease. World Health Organization, Geneva
Wright IC, Rabe-Hesketh S, Woodruff PW, David AS, Murray RM, Bullmore ET (2000) Meta-analysis of regional brain volumes in schizophrenia. Am J Psychiatry 157:16–25
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kutuk, M.S., Ozgun, M.T., Uludag, S. et al. Postnatal outcome of isolated, nonprogressive, mild borderline fetal ventriculomegaly. Childs Nerv Syst 29, 803–808 (2013). https://doi.org/10.1007/s00381-013-2020-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-013-2020-0