Abstract
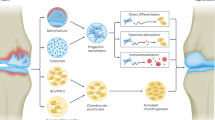
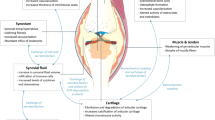
Osteoarthritis (OA) is a disease of the entire joint. Different treatment strategies for OA have been proposed and tested clinically without the desired efficacy. One reason for the scarcity of current chondroprotective agents may be the insufficient understanding of the patho-physiology of the joint and whether the joint damage is reversible or irreversible. In this review, we compile emerging data on cellular and pathological aspects of OA, and ask whether these data could give clue to when cartilage degradation is reversible and whether a point-of-no-return exists. We highlight different stages of OA, and speculate whether different intervention strategies (e.g. DMOAD vs. SMOADs) may only be efficacious at distinct stages of OA.




Similar content being viewed by others
Abbreviations
- ADAMTS:
-
A disintegrin and metalloproteinase with thrombospondin motifs
- BMP:
-
Bone morphogenetic protein
- CTX:
-
C-terminal telopeptide fragments
- DMOAD:
-
Disease modifying OA drug
- ECM:
-
Extracellular matrix
- FGF:
-
Fibroblast growth factor
- IGF-1:
-
Insulin growth factor
- JSW:
-
Joint space width
- MMP:
-
Matrix metalloproteinases
- OA:
-
Osteoarthritis
- OPG:
-
Osteoprotegerin
- PTH:
-
Parathyroid hormone
- RA:
-
Rheumatoid arthritis
- RANKL:
-
Receptor activator for nuclear factor κ B ligand
- SMOAD:
-
Structure modifying OA drug
- TGF:
-
Tissue growth factor
References
Kleemann RU, Krocker D, Cedraro A, Tuischer J, Duda GN (2005) Altered cartilage mechanics and histology in knee osteoarthritis: relation to clinical assessment (ICRS Grade). Osteoarthr Cartil 13:963–985
Felson DT, Neogi T (2004) Osteoarthritis: is it a disease of cartilage or of bone? Arthritis Rheum 50:341–344
Hayami T, Pickarski M, Wesolowski GA et al (2004) The role of subchondral bone remodeling in osteoarthritis: reduction of cartilage degeneration and prevention of osteophyte formation by alendronate in the rat anterior cruciate ligament transection model. Arthritis Rheum 50:1193–1206
Karsdal MA, Leeming DJ, Dam EB et al (2008) Should subchondral bone turnover be targeted when treating osteoarthritis? Osteoarthr Cartil 16:638–646
Hayami T, Pickarski M, Zhuo Y, Wesolowski GA, Rodan GA, Duong lT (2006) Characterization of articular cartilage and subchondral bone changes in the rat anterior cruciate ligament transection and meniscectomized models of osteoarthritis 2. Bone 38:234–243
Oestergaard S, Rasmussen KE, Doyle N et al (2008) Evaluation of cartilage and bone degradation in a murine collagen antibody-induced arthritis model. Scand J Immunol 67:304–312
Christgau S, Tanko LB, Cloos PA et al (2004) Suppression of elevated cartilage turnover in postmenopausal women and in ovariectomized rats by estrogen and a selective estrogen-receptor modulator (SERM). Menopause 11:508–518
Bagger YZ, Tanko LB, Alexandersen P et al (2005) Oral salmon calcitonin induced suppression of urinary collagen type II degradation in postmenopausal women: a new potential treatment of osteoarthritis. Bone 37:425–430
Karsdal MA, Leeming DJ, Byrjalsen I, Christiansen C (2008) Tibolone inhibits bone resorption without secondary positive effects on cartilage degradation. BMC Musculoskelet Disord 9:153
Martel-Pelletier J, Cloutier JM, Pelletier JP (1990) Cathepsin B and cysteine protease inhibitors in human osteoarthritis. J Orthop Res 8:336–344
Edwards JC (2000) Fibroblast biology. Development and differentiation of synovial fibroblasts in arthritis. Arthritis Res 2:344–347
Martin TJ, Quinn JM, Gillespie MT, Ng KW, Karsdal MA, Sims NA (2006) Mechanisms involved in skeletal anabolic therapies. Ann N Y Acad Sci 1068:458–470
Kong YY, Yoshida H, Sarosi I et al (1999) OPGL is a key regulator of osteoclastogenesis, lymphocyte development and lymph-node organogenesis. Nature 397:315–323
Karsdal MA, Martin TJ, Bollerslev J, Christiansen C, Henriksen K (2007) Are nonresorbing osteoclasts sources of bone anabolic activity? J Bone Miner Res 22:487–494
Karsdal MA, Neutzsky-Wulff AV, Dziegiel MH, Christiansen C, Henriksen K (2008) Osteoclasts secrete non-bone derived signals that induce bone formation. Biochem Biophys Res Commun 366:483–488
Massicotte F, Aubry I, Martel-Pelletier J, Pelletier JP, Fernandes J, Lajeunesse D (2006) Abnormal insulin-like growth factor 1 signaling in human osteoarthritic subchondral bone osteoblasts 12. Arthritis Res Ther 8:R177
Henrotin Y, Reginster JY (1999) Anabolic events in osteoarthritis 5. Osteoarthr Cartil 7:310–312
Aigner T, Kurz B, Fukui N, Sandell L (2002) Roles of chondrocytes in the pathogenesis of osteoarthritis. Curr Opin Rheumatol 14:578–584
Goldring MB (2006) Update on the biology of the chondrocyte and new approaches to treating cartilage diseases. Best Pract Res Clin Rheumatol 20:1003–1025
Valcourt U, Gouttenoire J, Aubert-Foucher E, Herbage D, Mallein-Gerin F (2003) Alternative splicing of type II procollagen pre-mRNA in chondrocytes is oppositely regulated by BMP-2 and TGF-[beta]1. FEBS Lett 545:115–119
Pfander D, Swoboda B, Kirsch T (2001) Expression of early and late differentiation markers (proliferating cell nuclear antigen, Syndecan-3, Annexin VI, and Alkaline Phosphatase) by human osteoarthritic chondrocytes. Am J Pathol 159:1777–1783
Reimann I, Mankin HJ, Trahan C (1977) Quantitative histologic analyses of articular cartilage and subchondral bone from osteoarthritic and normal human hips. Acta Orthop Scand 48:63–73
Kronenberg HM (2003) Developmental regulation of the growth plate. Nature 423:332–336
Kamekura S, Kawasaki Y, Hoshi K et al (2006) Contribution of runt-related transcription factor 2 to the pathogenesis of osteoarthritis in mice after induction of knee joint instability. Arthritis Rheum 54:2462–2470
Kawaguchi H (2008) Endochondral ossification signals in cartilage degradation during osteoarthritis progression in experimental mouse models. Mol Cells 25:1–6
Yu L, Liu H, Yan M et al (2007) Shox2 is required for chondrocyte proliferation and maturation in proximal limb skeleton. Dev Biol 306:549–559
Tew SR, Clegg PD, Brew CJ, Redmond CM, Hardingham TE (2007) SOX9 transduction of a human chondrocytic cell line identifies novel genes regulated in primary human chondrocytes and in osteoarthritis. Arthritis Res Ther 9:R107
Akiyama H, Chaboissier MC, Martin JF, Schedl A, de CB (2002) The transcription factor Sox9 has essential roles in successive steps of the chondrocyte differentiation pathway and is required for expression of Sox5 and Sox6. Genes Dev 16:2813–2828
Aigner T, Gebhard PM, Schmid E, Bau B, Harley V, Poschl E (2003) SOX9 expression does not correlate with type II collagen expression in adult articular chondrocytes. Matrix Biol 22:363–372
Schaller S, Henriksen K, Hoegh-Andersen P et al (2005) In vitro, ex vivo, and in vivo methodological approaches for studying therapeutic targets of osteoporosis and degenerative joint diseases: how biomarkers can assist? Assay Drug Dev Technol 3:553–580
Charni-Ben TN, Garnero P (2007) Monitoring cartilage turnover. Curr Rheumatol Rep 9:16–24
Cremers S, Bilezikian JP, Garnero P (2008) Bone markers—new aspects. Clin Lab 54:461–471
Karsdal MA, Madsen SH, Christiansen C, Henriksen K, Fosang AJ, Sondergaard BC (2008) Cartilage degradation is fully reversible in the presence of aggrecanase but not matrix metalloproteinase activity. Arthritis Res Ther 10:R63
van Meurs JB, van Lent PL, Holthuysen AE, Singer II, Bayne EK, van den Berg WB (1999) Kinetics of aggrecanase- and metalloproteinase-induced neoepitopes in various stages of cartilage destruction in murine arthritis. Arthritis Rheum 42:1128–1139
Karsdal MA, Henriksen K, Sorensen MG et al (2005) Acidification of the osteoclastic resorption compartment provides insight into the coupling of bone formation to bone resorption. Am J Pathol 166:467–476
Behrens F, Kraft EL, Oegema TR Jr (1989) Biochemical changes in articular cartilage after joint immobilization by casting or external fixation. J Orthop Res 7:335–343
Sondergaard BC, Henriksen K, Wulf H et al (2006) Relative contribution of matrix metalloprotease and cysteine protease activities to cytokine-stimulated articular cartilage degradation. Osteoarthr Cartil 14:738–748
Karsdal MA, Sumer EU, Wulf H et al (2007) Induction of increased cAMP levels in articular chondrocytes blocks matrix metalloproteinase-mediated cartilage degradation, but not aggrecanase-mediated cartilage degradation. Arthritis Rheum 56:1549–1558
Mohtai M, Smith RL, Schurman DJ et al (1993) Expression of 92-kD type IV collagenase/gelatinase (gelatinase B) in osteoarthritic cartilage and its induction in normal human articular cartilage by interleukin 1. J Clin Invest 92:179–185
Dean DD, Martel-Pelletier J, Pelletier JP, Howell DS, Woessner JF Jr (1989) Evidence for metalloproteinase and metalloproteinase inhibitor imbalance in human osteoarthritic cartilage. J Clin Invest 84:678–685
Stoop R, van der Kraan PM, Buma P, Hollander AP, Poole AR, van den Berg WB (1999) Denaturation of type II collagen in articular cartilage in experimental murine arthritis. Evidence for collagen degradation in both reversible and irreversible cartilage damage. J Pathol 188:329–337
Acknowledgments
We would like to thank our colleagues at Nordic Bioscience for their participation in inspirational discussions. We would also like to thank several of our fellow scientist, which we have continues discussion with at meetings and seminars.
Conflict of interest
The authors are not aware of any conflict of interest pertaining to this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bay-Jensen, AC., Hoegh-Madsen, S., Dam, E. et al. Which elements are involved in reversible and irreversible cartilage degradation in osteoarthritis?. Rheumatol Int 30, 435–442 (2010). https://doi.org/10.1007/s00296-009-1183-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-009-1183-1