Abstract
Objective
Gastroesophageal reflux disease (GERD) symptoms are commonly reported in primary hyperparathyroidism (pHPT). Although a calcium-mediated cause-and-effect relationship has been suggested, it remains unknown if parathyroidectomy improves GERD symptoms.
Methods
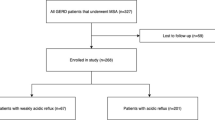
Over a 22-month period, 1,175 (39 %) of 3,000 consecutive adult patients with pHPT and symptomatic GERD (on prescription reflux medications daily for ≥2 years) undergoing parathyroidectomy were entered into a prospective study. Standardized Frequency Scale for Symptoms of GERD (FSSG) questionnaire was used to assess symptoms before, 1 and 2 years after parathyroidectomy.
Results
Daily prescription medication was used by 81 %, while 19 % used daily non-prescription drugs, both for a mean of 2.9 ± 0.7 years. GERD symptoms improved (26 %) or resolved completely (36 %) in 62 % of patients (p < 0.0001 vs. preoperative baseline) 1 year after parathyroidectomy. Prescription medications for GERD decreased from 81 % of enrolled patients to 26 % (p < 0.0001) 12 months postoperatively, with 39 % having complete symptom relief and taking no medications (p < 0.0001). Daily use of prescription GERD medications decreased to occasional over-the-counter drug use in 35 % after parathyroidectomy (p < 0.0001). Mean FSSG scores decreased significantly postoperatively (pre-op: 18.0 ± 8.0 vs. post-op: 10.0 ± 5.0; p < 0.0001), with significant improvements in all 12 FSSG categories, including motility (pre-op: 7.3 ± 3.0 vs. post-op: 4.4 ± 3.0; p < 0.0001) and acid reflux symptoms (pre-op: 10.8 ± 5.0 vs. post-op: 5.9 ± 4.0; p < 0.0001). Symptomatic improvements were durable 2 years after parathyroidectomy.
Conclusion
Symptomatic GERD is common in pHPT. Parathyroidectomy provides significant, durable relief of both motility and acid reflux symptoms allowing discontinuation of prescription drug use for GERD in most (74 %) patients providing yet another indication for parathyroidectomy in pHPT.






Similar content being viewed by others
Abbreviations
- pHPT:
-
Primary hyperparathyroidism
- FSSG:
-
Frequency Scale for Symptoms of Gastroesophageal Reflux
- GERD:
-
Gastroesophageal reflux disease
- IRB:
-
Institutional review board
- QOL:
-
Quality of life
References
Weber T, Eberle J, Messelhäuser U, Schiffmann L, Nies C, Schabram J, Zielke A, Holzer K, Rottler E, Henne-Bruns D, Keller M, von Wietersheim J (2013) Parathyroidectomy, elevated depression scores, and suicidal ideation in patients with primary hyperparathyroidism: results of a prospective multicenter study. JAMA Surg 148(2):109–115
Diniz ET, Bandeira F, Lins OG, Cavalcanti EN, de Arruda TM, Januário AM, Diniz KT, Marques TF, Azevedo H (2013) Primary hyperparathyroidism is associated with subclinical peripheral neural alterations. Endocr Pract 19(2):219–225
Reppe S, Stilgren L, Abrahamsen B, Olstad OK, Cero F, Brixen K, Nissen-Meyer LS, Gautvik KM (2007) Abnormal muscle and hematopoietic gene expression may be important for clinical morbidity in primary hyperparathyroidism. Am J Physiol Endocrinol Metab 292(5):E1465–E1473
Joborn C, Joborn H, Rastad J, Akerström G, Ljunghall S (1988) Maximal isokinetic muscle strength in patients with primary hyperparathyroidism before and after parathyroid surgery. Br J Surg 75(1):77–80
Chan AK, Duh QY, Katz MH, Siperstein AE, Clark OH (1995) Clinical manifestations of primary hyperparathyroidism before and after parathyroidectomy. A case–control study. Ann Surg 402(12):412–414
Gardner EC, Hersh T (1981) Primary hyperparathyroidism and the gastrointestinal tract. South Med J 74(2):197–199
Abboud B, Daher R, Boujaoude J (2011) Digestive manifestations of parathyroid disorders. World J Gastroenterol 17(36):4063–4066
Peery AF, Dellon ES, Lund J, Crockett SD, McGowan CE, Bulsiewicz WJ, Gangarosa LM, Thiny MT, Stizenberg K, Morgan DR, Ringel Y, Kim HP, Dibonaventura MD, Carroll CF, Allen JK, Cook SF, Sandler RS, Kappelman MD, Shaheen NJ (2012) Burden of gastrointestinal disease in the United States: 2012 update. Gastroenterology 143(5):1179–1187
Toghanian S, Johnson DA, Stålhammar NO, Zerbib F (2011) Burden of gastro-oesophageal reflux disease in patients with persistent and intense symptoms despite proton pump inhibitor therapy: a post hoc analysis of the 2007 national health and wellness survey. Clin Drug Investig 31(10):703–715
Sandler RS, Everhart JE, Donowitz M, Adams E, Cronin K, Goodman C, Gemmen E, Shah S, Avdic A, Rubin R (2002) The burden of selected digestive diseases in the United States. Gastroenterology 122(27):1500–1511
Sawaya RA, Macgill A, Parkman HP, Friedenberg FK (2012) Use of the Montreal global definition as an assessment of quality of life in reflux disease. Dis Esophagus 25(6):477–483
Vakil N, van Zanten SV, Kahrilas P, Dent J, Jones R (2007) Globale Konsensusgruppe. The Montreal definition and classification of gastroesophageal reflux disease: a global, evidence-based consensus paper]. Gastroenterology 45(11):1125–1140
Holtmann G, Chassany O, Devault KR, Schmitt H, Gebauer U, Doerfler H, Malagelada JR (2009) International validation of a health-related quality of life questionnaire in patients with erosive gastro-oesophageal reflux disease. Aliment Pharmacol Ther 29(6):615–625
Chassany O, Holtmann G, Malagelada J, Gebauer U, Doerfler H, Devault K (2008) Systematic review: health-related quality of life (HRQOL) questionnaires in gastro-oesophageal reflux disease. Aliment Pharmacol Ther 27(11):1053–1070
Kusano M, Shimoyama Y, Sugimoto S, Kawamura O, Maeda M, Minashi K, Kuribayashi S, Higuchi T, Zai H, Ino K, Horikoshi T, Sugiyama T, Toki M, Ohwada T, Mori M (2004) Development and evaluation of FSSG: frequency scale for the symptoms of GERD. J Gastroenterol 39(9):888–891
Danjo A, Yamaguchi K, Fujimoto K, Saitoh T, Inamori M, Ando T, Shimatani T, Adachi K, Kinjo F, Kuribayashi S, Mitsufuji S, Fujiwara Y, Koyama S, Akiyama J, Takagi A, Manabe N, Miwa H, Shimoyama Y, Kusano M (2009) Comparison of endoscopic findings with symptom assessment systems (FSSG and QUEST) for gastroesophageal reflux disease in Japanese centres. J Gastroenterol Hepatol 24(4):633–638
Norman J, Lopez J, Politz D (2012) Abandoning unilateral parathyroidectomy: why we reversed our position after 15,000 parathyroid operations. J Am Coll Surg 214(3):260–269
Goodman A, Politz D, Lopez J, Norman J (2011) Intrathyroid parathyroid adenoma: incidence and location—the case against thyroid lobectomy. Otolaryngol Head Neck Surg 144(6):867–871
Reiher AE, Mazeh H, Schaefer S, Gould J, Chen H, Sippel RS (2012) Symptoms of gastroesophageal reflux disease improve after parathyroidectomy. Surgery 152(6):1232–1237
Edwards ME, Rotramel A, Beyer T, Gaffud MJ, Djuricin G, Loviscek K, Solorzano CC, Prinz RA (2006) Improvement in the health-related quality-of-life symptoms of hyperparathyroidism is durable on long-term follow-up. Surgery 140(4):655–663 (discussion 653–654)
Pasieka JL, Parsons L, Jones J (2009) The long-term benefit of parathyroidectomy in primary hyperparathyroidism: a 10-year prospective surgical outcome study. Surgery 146(6):1006–1013. doi:10.1016/j.surg.2009.10.021
Melck AL, Armstrong MJ, Stang MT, Carty SE, Yip L (2010) Medication discontinuation after curative surgery for sporadic primary hyperparathyroidism. Surgery 148(6):1113–1118 (discussion 1118–1119)
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Norman, J., Politz, D., Lopez, J. et al. Surgical Cure of Primary Hyperparathyroidism Ameliorates Gastroesophageal Reflux Symptoms. World J Surg 39, 706–712 (2015). https://doi.org/10.1007/s00268-014-2876-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-014-2876-5