Abstract
Background
Osteomyelitis is a challenging diagnosis for clinicians, particularly in very young children. At our institution, the magnetic resonance imaging (MRI) protocol in suspected osteomyelitis for children 5 years of age or younger includes a large field of imaging regardless of the clinical site of concern.
Objective
To determine if extended field of view (FOV) MRI contributes important information in young children with suspected osteomyelitis.
Materials and methods
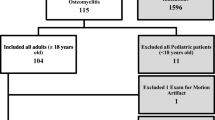
A retrospective study was performed including children 5 years of age or younger with suspected osteomyelitis from January 2011 to September 2015. All children underwent coronal fluid-sensitive MRI from neck to feet. Focused imaging was performed as necessary on abnormal sites depicted on survey imaging. Two radiologists reviewed the imaging findings, which were compared to the clinical outcome.
Results
We studied 51 children with a mean age of 2.2 years (range: 21 days-5.5 years); 53% were boys. Osteomyelitis was depicted by MRI in 20 subjects (39.2%). Survey coronal fluid-sensitive imaging was accomplished by adding a single fluid-sensitive series in 1 child, 2 series in 31 children, 3 series in 16 children and 4 series in 3 children. Survey imaging added a median total time of 6:51 min to the examination (range: 2.29–20.54 min). Extended FOV imaging added important information in 11/51 subjects (21.6%), in 6 cases (11.8%) of infection and in 5 cases (9.8%) by suggesting alternative diagnoses.
Conclusion
The addition of extended FOV MRI in young children with suspected osteomyelitis added important clinical information in 21.6% of patients while only adding a median of 6:51 min to the examination. It is our experience that in children ≤5 years of age with suspected osteomyelitis, extended FOV imaging adds important information and may result in changes in management.







Similar content being viewed by others
References
Browne LP, Guillerman RP, Orth RC et al (2012) Community-acquired staphylococcal musculoskeletal infection in infants and young children: necessity of contrast-enhanced MRI for the diagnosis of growth cartilage involvement. AJR Am J Roentgenol 198:194–199
Gafur OA, Copley LA, Hollmig ST et al (2008) The impact of the current epidemiology of pediatric musculoskeletal infection on evaluation and treatment guidelines. J Pediatr Orthop 28:777–785
Jaramillo D (2011) Infection: musculoskeletal. Pediatr Radiol 41:S127–S134
Jaramillo D, Dormans JP, Delgado J et al (2017) Hematogenous osteomyelitis in infants and children: imaging of a changing disease. Radiology 283:629–643
Guillerman RP (2013) Osteomyelitis and beyond. Pediatr Radiol 43:S193–S203
Yeo A, Ramachandran M (2014) Acute haematogenous osteomyelitis in children. BMJ 348:g66
Riise OR, Kirkhus E, Handeland KS et al (2008) Childhood osteomyelitis-incidence and differentiation from other acute onset musculoskeletal features in a population-based study. BMC Pediatr 8:45
Metwalli ZA, Kan JH, Munjal KA et al (2013) MRI of suspected lower extremity musculoskeletal infection in the pediatric patient: how useful is bilateral imaging? AJR Am J Roentgenol 201:427–432
Asmar BI (1992) Osteomyelitis in the neonate. Infect Dis Clin N Am 6:117–132
Howman-Giles R, Uren R (1992) Multifocal osteomyelitis in childhood. Review by radionuclide bone scan. Clin Nucl Med 17:274–278
Labbe JL, Peres O, Leclair O et al (2010) Acute osteomyelitis in children: the pathogenesis revisited? Orthop Traumatol Surg Res 96:268–275
Mathias B, Mira JC, Larson SD (2016) Pediatric sepsis. Curr Opin Pediatr 28:380–387
Browne LP, Mason EO, Kaplan SL et al (2008) Optimal imaging strategy for community-acquired Staphylococcus aureus musculoskeletal infections in children. Pediatr Radiol 38:841–847
Monsalve J, Kan JH, Schallert EK et al (2015) Septic arthritis in children: frequency of coexisting unsuspected osteomyelitis and implications on imaging work-up and management. AJR Am J Roentgenol 204:1289–1295
Peltola H, Paakkonen M (2014) Acute osteomyelitis in children. N Engl J Med 370:352–360
Yagupsky P, Porsch E, St Geme JW 3rd (2011) Kingella kingae: an emerging pathogen in young children. Pediatrics 127:557–565
Sreenivas T, Nataraj AR, Menon J, Patro DK (2011) Acute multifocal haematogenous osteomyelitis in children. J Child Orthop 5:231–235
Mika J, Schleicher I, Gerlach U et al (2012) Primary bone lymphomas thought to be osteomyelitis urgently demand a rapid diagnosis in bone pathology. Anticancer Res 32:4905–4912
McCarville MB, Chen JY, Coleman JL et al (2015) Distinguishing osteomyelitis from Ewing sarcoma on radiography and MRI. AJR Am J Roentgenol 205:640–650
McCarville MB (2009) The child with bone pain: malignancies and mimickers. Cancer Imaging 9:S115–S121
Lee HJ, Kim MK, Yun KW et al (2014) Lymphoma with unusual manifestations resembling acute osteomyelitis in bilateral ankles of an 8-year-old boy: a case report. J Pediatr Orthop B 23:139–143
Henninger B, Glodny B, Rudisch A et al (2013) Ewing sarcoma versus osteomyelitis: differential diagnosis with magnetic resonance imaging. Skelet Radiol 42:1097–1104
Harknett KM, Hussain SK, Rogers MK, Patel NC (2014) Scurvy mimicking osteomyelitis: case report and review of the literature. Clin Pediatr (Phila) 53:995–999
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lindsay, A.J., Delgado, J., Jaramillo, D. et al. Extended field of view magnetic resonance imaging for suspected osteomyelitis in very young children: is it useful?. Pediatr Radiol 49, 379–386 (2019). https://doi.org/10.1007/s00247-018-4317-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-018-4317-3