Abstract
Background
The presence of a hernia sac in congenital diaphragmatic hernia (CDH) has been reported to be associated with higher lung volumes and better postnatal outcomes.
Objective
To compare prenatal imaging (ultrasound and MRI) prognostic measurements and postnatal outcomes of CDH with and without hernia sac.
Materials and methods
We performed database searches from January 2008 to March 2017 for surgically proven cases of CDH with and without hernia sac. All children had a detailed ultrasound (US) examination and most had an MRI examination. We reviewed the medical records of children enrolled in our Pulmonary Hypoplasia Program.
Results
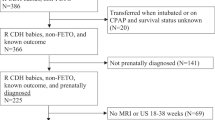
Of 200 cases of unilateral CDH, 46 (23%) had hernia sacs. Cases of CDH with hernia sac had a higher mean lung-to-head ratio (LHR; 1.61 vs. 1.17; P<0.01), a higher mean observed/expected LHR (0.49 vs. 0.37; P<0.01), and on MRI a higher mean observed/expected total lung volume (0.53 vs. 0.41; P<0.01). Based on a smooth interface between lung and herniated contents, hernia sac or eventration was prospectively questioned by US and MRI in 45.7% and 38.6% of cases, respectively. Postnatally, hernia sac is associated with shorter median periods of admission to the neonatal intensive care unit (45.0 days vs. 61.5 days, P=0.03); mechanical ventilation (15.5 days vs. 23.5 days, P=0.04); extracorporeal membrane oxygenation (251 h vs. 434 h, P=0.04); decreased rates of patch repair (39.0% vs. 69.2%, P<0.01); and pulmonary hypertension (56.1% vs. 75.4%, P=0.03).
Conclusion
Hernia sac is associated with statistically higher prenatal prognostic measurements and improved postnatal outcomes. Recognition of a sharp interface between lung and herniated contents may allow for improved prenatal diagnosis; however, delivery and management should still occur at experienced quaternary neonatal centers.



Similar content being viewed by others
References
Langham M, Kays D, Ledbetter D et al (1996) Congenital diaphragmatic hernia. Epidemiology and outcome. Clin Perinatol 23:671–687
Beresford MW, Shaw NJ (2000) Outcome of congenital diaphragmatic hernia. Pediatr Pulmonol 30:249–256
Mah VK, Zamakhshary M, Mah DY et al (2009) Absolute vs relative improvements in congenital diaphragmatic hernia survival: what happened to “hidden mortality.” J Pediatr Surg 44:877–882
Brownlee EM, Howatson AG, Davis CF, Sabharwal AJ (2009) The hidden mortality of congenital diaphragmatic hernia: a 20-year review. J Pediatr Surg 44:317–320
Peralta CFA, Cavoretto P, Csapo B et al (2005) Assessment of lung area in normal fetuses at 12-32 weeks. Ultrasound Obstet Gynecol 26:718–724
Jani J, Keller RL, Benachi A et al (2006) Prenatal prediction of survival in isolated left-sided diaphragmatic hernia. Ultrasound Obstet Gynecol 27:18–22
Jani J, Nicolaides KH, Keller RL et al (2007) Observed to expected lung area to head circumference ratio in the prediction of survival in fetuses with isolated diaphragmatic hernia. Ultrasound Obstet Gynecol 30:67–71
Jani J, Cannie M, Sonigo P et al (2008) Value of prenatal magnetic resonance imaging in the prediction of postnatal outcome in fetuses with diaphragmatic hernia. Ultrasound Obstet Gynecol 32:793–799
Spaggiari E, Stirnemann J, Bernard JP et al (2013) Prognostic value of a hernia sac in congenital diaphragmatic hernia. Ultrasound Obstet Gynecol 41:286–290
Zamora IJ, Cass DL, Lee TC et al (2013) The presence of a hernia sac in congenital diaphragmatic hernia is associated with better fetal lung growth and outcomes. J Pediatr Surg 48:1165–1171
Victoria T, Jaramillo D, Roberts TPL et al (2014) Fetal magnetic resonance imaging: jumping from 1.5 to 3 tesla (preliminary experience). Pediatr Radiol 44:376–386
Victoria T, Johnson AM, Edgar JC et al (2016) Comparison between 1.5-T and 3-T MRI for fetal imaging: Is there an advantage to imaging with a higher field strength? AJR Am J Roentgenol 206:195–201
Metkus AP, Filly RA, Stringer MD et al (1996) Sonographic predictors of survival in fetal diaphragmatic hernia. J Pediatr Surg 31:148–151
DeKoninck P, Gratacos E, Van Mieghem T et al (2011) Results of fetal endoscopic tracheal occlusion for congenital diaphragmatic hernia and the set up of the randomized controlled TOTAL trial. Early Hum Dev 87:619–624
Mehollin-Ray AR, Cassady CI, Cass DL, Olutoye OO (2012) Fetal MR imaging of congenital diaphragmatic hernia. Radiographics 32:1067–1084
Rypens F, Metens T, Rocourt N et al (2001) Fetal lung volume: estimation at MR imaging-initial results. Radiology 219:236–241
Ward VL, Nishino M, Hatabu H et al (2006) Fetal lung volume measurements: determination with MR imaging — effect of various factors. Radiology 240:187–193
Grizelj R, Bojanić K, Vuković J et al (2017) Hernia sac presence portends better survivability of isolated congenital diaphragmatic hernia with “liver-up.” Am J Perinatol 34:515–519
Zamora IJ, Mehollin-Ray AR, Sheikh F et al (2015) Predictive value of MRI findings for the identification of a hernia sac in fetuses with congenital diaphragmatic hernia. AJR Am J Roentgenol 205:1121–1125
Acknowledgments
We thank Mr. Michael J. Kallan for his assistance with the statistical analyses in this study. Preliminary data were presented at the International Fetal Medicine and Surgery Society Annual Meeting on Oct. 9, 2017.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Oliver, E.R., DeBari, S.E., Adams, S.E. et al. Congenital diaphragmatic hernia sacs: prenatal imaging and associated postnatal outcomes. Pediatr Radiol 49, 593–599 (2019). https://doi.org/10.1007/s00247-018-04334-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-018-04334-9