Abstract
Introduction
The objective of the study was to determine whether tumor-associated neovascularization on high-resolution gadofosveset-enhanced magnetic resonance angiography (MRA) is a useful biomarker for predicting survival in patients with newly diagnosed glioblastomas.
Methods
Before treatment, 35 patients (25 men; mean age, 64 ± 14 years) with glioblastoma underwent MRI including first-pass dynamic susceptibility contrast (DSC) perfusion and post-contrast T1WI sequences with gadobutrol (0.1 mmol/kg) and, 48 h later, high-resolution MRA with gadofosveset (0.03 mmol/kg). Volumes of interest for contrast-enhancing lesion (CEL), non-CEL, and contralateral normal-appearing white matter were obtained, and DSC perfusion and DWI parameters were evaluated. Prognostic factors were assessed by Kaplan-Meier survival and Cox proportional hazards model.
Results
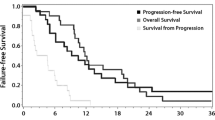
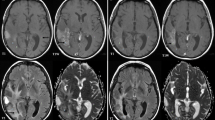
Eighteen (51.42 %) glioblastomas were hypervascular on high-resolution MRA. Hypervascular glioblastomas were associated with higher CEL volume and lower Karnofsky score. Median survival rates for patients with hypovascular and hypervascular glioblastomas treated with surgery, radiotherapy, and chemotherapy were 15 and 9.75 months, respectively (P < 0.001). Tumor-associated neovascularization was the best predictor of survival at 5.25 months (AUC = 0.794, 81.2 % sensitivity, 77.8 % specificity, 76.5 % positive predictive value, 82.4 % negative predictive value) and yielded the highest hazard ratio (P < 0.001).
Conclusions
Tumor-associated neovascularization detected on high-resolution blood-pool-contrast-enhanced MRA of newly diagnosed glioblastoma seems to be a useful biomarker that correlates with worse survival.


Similar content being viewed by others
References
Stupp R, Hegi M, Mason W et al (2009) Effects of radiotherapy with concomitant and adjuvant temozolomide versus radiotherapy alone on survival in glioblastoma in a randomised phase III study: 5-year analysis of the EORTC-NCIC trial. Lancet Oncol 10:459–466
Lamborn KR, Chang SM, Prados MD (2004) Prognostic factors for survival of patients with glioblastoma: recursive partitioning analysis. Neuro Oncol 6:227–235
Birner P, Piribauer M, Fischer I et al (2003) Vascular patterns in glioblastoma influence clinical outcome and associate with variable expression of angiogenic proteins: evidence for distinct angiogenic subtypes. Brain Pathol 13:133–143
Wesseling P, van der Laak JA, Link M, Teepen HL, Ruiter DJ (1998) Quantitative analysis of microvascular changes in diffuse astrocytic neoplasms with increasing grade of malignancy. Hum Pathol 29:352–358
Preusser M, Heinzl H, Gelpi E et al (2006) European Organization for Research and Treatment of Cancer Brain Tumor Group. Histopathologic assessment of hot-spot microvessel density and vascular patterns in glioblastoma: Poor observer agreement limits clinical utility as prognostic factors: a translational research project of the European Organization for Research and Treatment of Cancer Brain Tumor Group. Cancer 107:162–170
Soda Y, Myskiw C, Rommel A, Verma IM (2013) Mechanisms of neovascularization and resistance to anti-angiogenic therapies in glioblastoma multiforme. J Mol Med (Berl) 91:439–448
Norden AD, Drappatz J, Wen PY (2008) Novel anti-angiogenic therapies for malignant gliomas. Lancet Neurol 7:1152–1160
Kadota T, Nakagawa H, Kuroda C (1998) Malignant glioma. Evaluation with 3D time-of-flight MR angiography. Acta Radiol 39:227–232
Sugahara T, Korogi Y, Kochi M et al (1998) Correlation of MR imaging determined cerebral blood volume maps with histologic and angiographic determination of vascularity of gliomas. AJR Am J Roentgenol 171:1479–1486
Wetzel SG, Cha S, Law M et al (2002) Preoperative assessment of intracranial tumors with perfusion MR and a volumetric interpolated examination: a comparative study with DSA. AJNR Am J Neuroradiol 23:1767–1774
Russell SM, Elliott R, Forshaw D, Golfinos JG, Nelson PK, Kelly PJ (2009) Glioma vascularity correlates with reduced patient survival and increased malignancy. Surg Neurol 72:242–246
Aronen H, Gazit I, Louis D et al (1994) Cerebral blood volume maps of gliomas: comparison with tumor grade and histologic findings. Radiology 191:41–51
Boxerman JL, Schmainda KM, Weisskoff RM (2006) Relative cerebral blood volume maps corrected for contrast agent extravasation significantly correlate with glioma tumor grade, whereas uncorrected maps do not. AJNR Am J Neuroradiol 27:859–867
Le Bas J, Kremer S, Grand S et al (2000) NMR perfusion imaging: applications to the study of brain tumor angiogenesis. Bull Acad Natl Med 184:557–567
Mills SJ, Patankar TA, Haroon HA, Balériaux D, Swindell R, Jackson A (2006) Do cerebral blood volume and contrast transfer coefficient predict prognosis in human glioma? AJNR Am J Neuroradiol 27:853–858
Hirai T, Murakami R, Nakamura H et al (2008) Prognostic value of perfusion MR imaging of high-grade astrocytomas: long-term follow-up study. AJNR Am J Neuroradiol 29:1505–1510
Jain R, Narang J, Griffith B et al (2013) Prognostic vascular imaging biomarkers in high-grade gliomas: tumor permeability as an adjunct to blood volume estimates. Acad Radiol 20:478–485
Farooki A, Narra V, Brown J (2004) Gadofosveset (EPIX/Schering). Curr Opin Investig Drugs 5:967–976
Caravan P (2009) Protein-targeted gadolinium-based magnetic resonance imaging (MRI) contrast agents: design and mechanism of action. Acc Chem Res 42:851–862
Spuentrup E, Jacobs JE, Kleimann JF et al (2010) High spatial resolution and high contrast visualization of brain arteries and veins: impact of blood pool contrast agent and water-selective excitation imaging at 3T. Röfo 182:1097–1104
Puig J, Blasco G, Essig M et al (2013) Albumin-binding MR blood pool contrast agent improves diagnostic performance in human brain tumour: comparison of two contrast agents for glioblastoma. Eur Radiol 23:1093–1101
Ronning PA, Helseth E, Meling TR, Johannesen TB (2012) A population-based study on the effect of temozolomide in the treatment of glioblastoma multiforme. Neuro Oncol 14:1178–1184
Pope WB, Sayre J, Perlina A, Villablanca JP, Mischel PS, Cloughesy TF (2005) MR imaging correlates of survival in patients with high-grade gliomas. AJNR Am J Neuroradiol 26:2466–2474
Calcagno V, de Mazancourt C (2010) Glmulti: An R Package for Easy Automated Model Selection with (Generalized) Linear Models. J Stat Softw 34 issue 12. http://www.jstatsoft.org/v34/i12
Cha S (2006) Update on brain tumor imaging: from anatomy to physiology. AJNR Am J Neuroradiol 27:475–487
Furnari FB, Fenton T, Bachoo RM et al (2007) Malignant astrocytic glioma: genetics, biology, and paths to treatment. Genes Dev 21:2683–2710
Lutz K, Wiestler B, Graf M et al (2014) Infiltrative patterns of glioblastoma: Identification of tumor progress using apparent diffusion coefficient histograms. J Magn Reson Imaging 39:1096–1103
Lev MH, Ozsunar Y, Henson JW, Rasheed AA, Barest GD, Harsh GR 4th et al (2004) Glial tumor grading and outcome prediction using dynamic spin-echo MR susceptibility mapping compared with conventional contrast-enhanced MR: confounding effect of elevated rCBV of oligodendrogliomas. AJNR Am J Neuroradiol 25:214–221
Jouanneau E (2008) Angiogenesis and gliomas: current issues and development of surrogate markers. Neurosurgery 62:31–50
Hardee ME, Zagzag D (2012) Mechanisms of glioma-associated neovascularization. Am J Pathol 181:1126–1141
Takano S (2012) Glioblastoma angiogenesis: VEGF resistance solutions and new strategies based on molecular mechanisms of tumor vessel formation. Brain Tumor Pathol 29:73–86
Jain R, Gutierrez J, Narang J et al (2011) In vivo correlation of tumor blood volume and permeability with histological and molecular angiogenic markers in gliomas. AJNR Am J Neuroradiol 32:388–394
Bullitt E, Gerig G, Pizer SM, Lin W, Aylward SR (2003) Measuring tortuosity of the intracerebral vasculature from MRA images. IEEE Trans Med Imaging 22:1163–1171
Jain RK (2001) Normalizing tumor vasculature with antiangiogenic therapy: a new paradigm for combination therapy. Nat Med 7:987–989
Yan K, Yang K, Rich JN (2013) The evolving landscape of glioblastoma stem cells. Curr Opin Neurol 26:701–707
Varallyay CG, Muldoon LL, Gahramanov S et al (2009) Dynamic MRI using iron oxide nanoparticles to assess early vascular effects of antiangiogenic versus corticosteroid treatment in a glioma model. J Cereb Blood Flow Metab 29:853–860
Varallyay CG, Nesbit E, Fu R et al (2013) High-resolution steady-state cerebral blood volume maps in patients with central nervous system neoplasms using ferumoxytol, a superparamagnetic iron oxide nanoparticle. J Cereb Blood Flow Metab 33:780–786
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical standards and patient consent
We declare that all human studies have been approved by the local Ethics Committee of Hospital Universitari Dr Josep Trueta in Girona and have therefore been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. We declare that all patients gave informed consent prior to inclusion in this study.
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Puig, J., Blasco, G., Daunis-i-Estadella, J. et al. High-resolution blood-pool-contrast-enhanced MR angiography in glioblastoma: tumor-associated neovascularization as a biomarker for patient survival. A preliminary study. Neuroradiology 58, 17–26 (2016). https://doi.org/10.1007/s00234-015-1599-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-015-1599-0