Abstract
Purpose
The pivotal trials for stroke prevention in non-valvular atrial fibrillation (NVAF) compared rivaroxaban, dabigatran, and apixaban with warfarin, as did most claims-based studies. Comparisons with phenprocoumon, the most frequently used vitamin K antagonist (VKA) in Germany, are scarce.
Methods
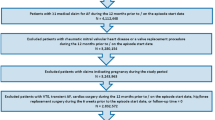
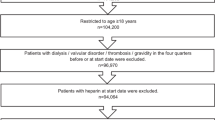
Risk of bleeding, ischemic stroke, and all-cause mortality in patients with NVAF were analyzed using data for 2010 to 2014 from a large German claims database. New users of oral anticoagulants from January 2012 to December 2013 were included and observed over 1 year. Baseline characteristics were adjusted using propensity score matching and logistic regression. Several sensitivity analyses were carried out.
Results
Fifty-nine thousand four hundred forty-nine rivaroxaban, 23,654 dabigatran, 4894 apixaban, and 87,997 matched phenprocoumon users were included. Adjusted hazard ratios (95% confidence intervals) compared with phenprocoumon were as follows: hospitalized bleedings: rivaroxaban 1.04 (0.97; 1.11), dabigatran 0.87 (0.77; 0.98), and apixaban 0.65 (0.50; 0.86); ischemic stroke: rivaroxaban 1.05 (0.94; 1.17), dabigatran 1.14 (0.96; 1.35), and apixaban 1.84 (1.20; 2.84); all-cause mortality: rivaroxaban 1.17 (1.11; 1.22), dabigatran 1.04 (0.95; 1.13), and apixaban 1.14 (0.97; 1.34).
Conclusions
With rivaroxaban, no significant differences were observed compared to phenprocoumon with regard to hospitalized bleedings or ischemic strokes. Dabigatran was associated with fewer bleedings and a similar risk of ischemic strokes compared to phenprocoumon. Apixaban was also associated with fewer bleedings but was unexpectedly associated with more ischemic strokes, possibly reflecting selective prescribing. The association of rivaroxaban with higher all-cause mortality unrelated to bleedings or strokes has been described previously but remains to be explained.


Similar content being viewed by others
References
Hein L, Wille H (2017) Antithrombotika und Antihämorrhagika. In: Schwabe U, Paffrath D (eds) Arzneiverordnungs-Report 2017. Springer-Verlag, Berlin, pp 353–372
Southworth MR, Reichman ME, Unger EF (2013) Dabigatran and postmarketing reports of bleeding. N Engl J Med 368:1272–1274
Connolly SJ, Ezekowitz MD, Yusuf S, Eikelboom J, Oldgren J, Parekh A, Pogue J, Reilly PA, Themeles E, Varrone J, Wang S, Alings M, Xavier D, Zhu J, Diaz R, Lewis BS, Darius H, Diener HC, Joyner CD, Wallentin L (2009) Dabigatran versus warfarin in patients with atrial fibrillation. N Engl J Med 361:1139–1151
Giugliano RP, Ruff CT, Braunwald E, Murphy SA, Wiviott SD, Halperin JL, Waldo AL, Ezekowitz MD, Weitz JI, Spinar J, Ruzyllo W, Ruda M, Koretsune Y, Betcher J, Shi M, Grip LT, Patel SP, Patel I, Hanyok JJ, Mercuri M, Antman EM, Investigators EA-T (2013) Edoxaban versus warfarin in patients with atrial fibrillation. N Engl J Med 369:2093–2104
Granger CB, Alexander JH, McMurray JJ, Lopes RD, Hylek EM, Hanna M, Al-Khalidi HR, Ansell J, Atar D, Avezum A, Bahit MC, Diaz R, Easton JD, Ezekowitz JA, Flaker G, Garcia D, Geraldes M, Gersh BJ, Golitsyn S, Goto S, Hermosillo AG, Hohnloser SH, Horowitz J, Mohan P, Jansky P, Lewis BS, Lopez-Sendon JL, Pais P, Parkhomenko A, Verheugt FW, Zhu J, Wallentin L (2011) Apixaban versus warfarin in patients with atrial fibrillation. N Engl J Med 365:981–992
Patel MR, Mahaffey KW, Garg J, Pan G, Singer DE, Hacke W, Breithardt G, Halperin JL, Hankey GJ, Piccini JP, Becker RC, Nessel CC, Paolini JF, Berkowitz SD, Fox KA, Califf RM (2011) Rivaroxaban versus warfarin in nonvalvular atrial fibrillation. N Engl J Med 365:883–891
Potpara TS, Lip GY (2017) Postapproval observational studies of non-vitamin K antagonist oral anticoagulants in atrial fibrillation. JAMA 317:1115–1116
Verhoef TI, Redekop WK, Daly AK, van Schie RM, de Boer A, Maitland-van der Zee AH (2014) Pharmacogenetic-guided dosing of coumarin anticoagulants: algorithms for warfarin, acenocoumarol and phenprocoumon. Br J Clin Pharmacol 77:626–641
Amin A, Deitelzweig S, Jing Y, Makenbaeva D, Wiederkehr D, Lin J, Graham J (2014) Estimation of the impact of warfarin's time-in-therapeutic range on stroke and major bleeding rates and its influence on the medical cost avoidance associated with novel oral anticoagulant use-learnings from ARISTOTLE, ROCKET-AF, and RE-LY trials. J Thromb Thrombolysis 38:150–159
Bjorck F, Renlund H, Lip GY, Wester P, Svensson PJ, Sjalander A (2016) Outcomes in a warfarin-treated population with atrial fibrillation. JAMA Cardiol 1:172–180
Le Heuzey JY, Ammentorp B, Darius H, De Caterina R, Schilling RJ, Schmitt J, Zamorano JL, Kirchhof P (2014) Differences among western European countries in anticoagulation management of atrial fibrillation. Data from the PREFER IN AF registry. Thromb Haemost 111:833–841
Leiria TL, Pellanda L, Miglioranza MH, Sant'anna RT, Becker LS, Magalhaes E, Lima GG (2010) Warfarin and phenprocoumon: experience of an outpatient anticoagulation clinic. Arq Bras Cardiol 94:41–45
Prochaska JH, Gobel S, Keller K, Coldewey M, Ullmann A, Lamparter H, Junger C, Al-Bayati Z, Baer C, Walter U, Bickel C, ten Cate H, Munzel T, Wild PS (2015) Quality of oral anticoagulation with phenprocoumon in regular medical care and its potential for improvement in a telemedicine-based coagulation service—results from the prospective, multi-center, observational cohort study thrombEVAL. BMC Med 13:14
Ruff CT, Giugliano RP, Braunwald E, Hoffman EB, Deenadayalu N, Ezekowitz MD, Camm AJ, Weitz JI, Lewis BS, Parkhomenko A, Yamashita T, Antman EM (2014) Comparison of the efficacy and safety of new oral anticoagulants with warfarin in patients with atrial fibrillation: a meta-analysis of randomised trials. Lancet 383:955–962
Wallentin L, Yusuf S, Ezekowitz MD, Alings M, Flather M, Franzosi MG, Pais P, Dans A, Eikelboom J, Oldgren J, Pogue J, Reilly PA, Yang S, Connolly SJ, investigators R-L (2010) Efficacy and safety of dabigatran compared with warfarin at different levels of international normalised ratio control for stroke prevention in atrial fibrillation: an analysis of the RE-LY trial. Lancet 376:975–983
Bai Y, Deng H, Shantsila A, Lip GY (2017) Rivaroxaban versus dabigatran or warfarin in real-world studies of stroke prevention in atrial fibrillation: systematic review and meta-analysis. Stroke 48:970–976
Romanelli RJ, Nolting L, Dolginsky M, Kym E, Orrico KB (2016) Dabigatran versus warfarin for atrial fibrillation in real-world clinical practice: a systematic review and meta-analysis. Circ Cardiovasc Qual Outcomes 9:126–134
Ntaios G, Papavasileiou V, Makaritsis K, Vemmos K, Michel P, Lip GYH (2017) Real-world setting comparison of nonvitamin-K antagonist oral anticoagulants versus vitamin-K antagonists for stroke prevention in atrial fibrillation: a systematic review and meta-analysis. Stroke 48:2494–2503
Hohnloser SH, Basic E, Nabauer M (2017) Comparative risk of major bleeding with new oral anticoagulants (NOACs) and phenprocoumon in patients with atrial fibrillation: a post-marketing surveillance study. Clin Res Cardiol 106:618–628
Hohnloser SH, Basic E, Hohmann C, Nabauer M (2018) Effectiveness and safety of non-vitamin K oral anticoagulants in comparison to phenprocoumon: data from 61,000 patients with atrial fibrillation. Thromb Haemost 118:526–538
Larsen TB, Skjoth F, Nielsen PB, Kjaeldgaard JN, Lip GY (2016) Comparative effectiveness and safety of non-vitamin K antagonist oral anticoagulants and warfarin in patients with atrial fibrillation: propensity weighted nationwide cohort study. BMJ 353:i3189
Nielsen PB, Skjoth F, Sogaard M, Kjaeldgaard JN, Lip GY, Larsen TB (2017) Effectiveness and safety of reduced dose non-vitamin K antagonist oral anticoagulants and warfarin in patients with atrial fibrillation: propensity weighted nationwide cohort study. BMJ 356:j510
AOK Bundesverband (2014) Zahlen und Fakten 2014. KomPart Verlagsgesellschaft, Berlin
Kuss O (2013) The z-difference can be used to measure covariate balance in matched propensity score analyses. J Clin Epidemiol 66:1302–1307
Bengtson LGS, Lutsey PL, Chen LY, MacLehose RF, Alonso A (2017) Comparative effectiveness of dabigatran and rivaroxaban versus warfarin for the treatment of non-valvular atrial fibrillation. J Cardiol 69:868–876
Coleman CI, Antz M, Ehlken B, Evers T (2016) REal-LIfe evidence of stroke prevention in patients with atrial fibrillation—the RELIEF study. Int J Cardiol 203:882–884
Graham DJ, Reichman ME, Wernecke M, Zhang R, Southworth MR, Levenson M, Sheu TC, Mott K, Goulding MR, Houstoun M, MaCurdy TE, Worrall C, Kelman JA (2015) Cardiovascular, bleeding, and mortality risks in elderly Medicare patients treated with dabigatran or warfarin for nonvalvular atrial fibrillation. Circulation 131:157–164
Staerk L, Fosbol EL, Lip GYH, Lamberts M, Bonde AN, Torp-Pedersen C, Ozenne B, Gerds TA, Gislason GH, Olesen JB (2017) Ischaemic and haemorrhagic stroke associated with non-vitamin K antagonist oral anticoagulants and warfarin use in patients with atrial fibrillation: a nationwide cohort study. Eur Heart J 38:907–915
Fox KA, Piccini JP, Wojdyla D, Becker RC, Halperin JL, Nessel CC, Paolini JF, Hankey GJ, Mahaffey KW, Patel MR, Singer DE, Califf RM (2011) Prevention of stroke and systemic embolism with rivaroxaban compared with warfarin in patients with non-valvular atrial fibrillation and moderate renal impairment. Eur Heart J 32:2387–2394
Ioannou A, Tsappa I, Metaxa S, Missouris CG (2017) Non-valvular atrial fibrillation: impact of apixaban on patient outcomes. Patient Relat Outcome Meas 8:121–131
Li XS, Deitelzweig S, Keshishian A, Hamilton M, Horblyuk R, Gupta K, Luo X, Mardekian J, Friend K, Nadkarni A, Pan X, Lip GYH (2017) Effectiveness and safety of apixaban versus warfarin in non-valvular atrial fibrillation patients in “real-world” clinical practice. A propensity-matched analysis of 76,940 patients. Thromb Haemost 117:1072–1082
Yao X, Abraham NS, Sangaralingham LR, Bellolio MF, McBane RD, Shah ND, Noseworthy PA (2016) Effectiveness and safety of dabigatran, rivaroxaban, and apixaban versus warfarin in nonvalvular atrial fibrillation. J Am Heart Assoc 5:e003725
Yao X, Shah ND, Sangaralingham LR, Gersh BJ, Noseworthy PA (2017) Non-vitamin K antagonist oral anticoagulant dosing in patients with atrial fibrillation and renal dysfunction. J Am Coll Cardiol 69:2779–2790
Boehringer Ingelheim Pharma GmbH & Co. KG (2011) Mitteilung an die Angehörigen der Heilberufe zur Bedeutung einer Überprüfung der Nierenfunktion von Patienten, die mit Pradaxa® (Dabigatranetexilat) behandelt werden. Rote-Hand-Brief vom 27. Oktober 2011
Acknowledgments
The authors would like to thank PD Dr. Michael von Brevern, Prof. Andreas Creutzig, Prof. Thomas Lempert, Prof. Wilhelm Niebling, and Dr. Birke Schneider for their advice on the study design and Prof. Oliver Kuss, University of Düsseldorf, for his helpful comments on propensity score matching, and Siobhan O’Leary for editing assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The study was supported by a grant to PMV forschungsgruppe by AOK Bundesverband for data analysis. J. Bleek and G. Schillinger are employed by the AOK Bundesverband; H. Schröder and A. Zawinell by the WIdO. PMV forschungsgruppe has received unrestricted grants—not related to the topic of DOAC—from health insurance funds (AOK Bundesverband, AOK Hessen, AOK Baden-Württemberg, BARMER), industry (Sanofi, Ferring), and public funding. The other authors declare no conflict of interest.
Electronic supplementary material
ESM 1
(PDF 718 kb)
Rights and permissions
About this article
Cite this article
Ujeyl, M., Köster, I., Wille, H. et al. Comparative risks of bleeding, ischemic stroke and mortality with direct oral anticoagulants versus phenprocoumon in patients with atrial fibrillation. Eur J Clin Pharmacol 74, 1317–1325 (2018). https://doi.org/10.1007/s00228-018-2504-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-018-2504-7