Abstract
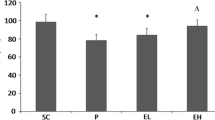
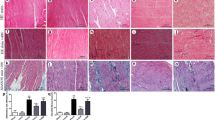
Qiliqiangxin (QL) can attenuate myocardial remodeling and improve cardiac function in some cardiac diseases, including heart failure and hypertension. This study was to explore the effects and mechanism of QL on atrial structural remodeling in atrial fibrillation (AF). Twenty-one rabbits were randomly divided into a sham-operation group, pacing group (pacing with 600 beats per minute for 4 weeks), and treatment group (2.5 g/kg/day). Before pacing, the rabbits received QL-administered p.o. for 1 week. We measured atrial electrophysiological parameters in all groups to evaluate AF inducibility and the atrial effective refractory period (AERP). Echocardiography evaluated cardiac function and structure. TUNEL detection, hematoxylin and eosin (HE) staining, and Masson’s trichrome staining were performed. Immunohistochemistry and western blotting (WB) were used to detect alterations in calcium channel L-type dihydropyridine receptor α2 subunit (DHPR) and fibrosis-related regulatory factors. AF inducibility was markedly decreased after QL treatment. Furthermore, we found that AERP and DHPR were reduced significantly in pacing rabbits compared with sham rabbits; treatment with QL increased DHPR and AERP compared to the pacing group. The QL group showed significantly decreased mast cell density and improved atrial ejection fraction values compared with the pacing group. Moreover, QL decreased interventricular septum thickness (IVSd) and left ventricular end-diastolic diameter (LVEDD). Compared with the sham group, the levels of TGFβ1 and P-smad2/3 were significantly upregulated in the pacing group. QL reduced TGF-β1 and P-smad2/3 levels and downstream fibrosis-related factors. Our study demonstrated that QL treatment attenuates atrial structural remodeling potentially by inhibiting TGF-β1/P-smad2/3 signaling pathway.





Similar content being viewed by others
References
Calkins H, Hindricks G, Cappato R et al (2017) 2017 HRS/EHRA/ECAS/APHRS/SOLAECE expert consensus statement on catheter and surgical ablation of atrial fibrillation. Heart Rhythm 14(10):e275–e444
Choi EK, Chang PC, Lee YS, Lin SF, Zhu W, Maruyama M, FishbeinMC CZ, Rubart-von der Lohe M, Field LJ, Chen PS (2012) Triggered firing and atrial fibrillation in transgenic mice with selective atrial fibrosis induced by overexpression of TGF-β1. Circ J 76(6):1354–1362
Fu H, Li G, Liu C, Li J, Wang X, Cheng L, Liu T (2015) Probucol prevents atrial remodeling by inhibiting oxidative stress and TNF- α/NF-κB/TGF-β signal transduction pathway in alloxan-induced diabetic rabbits. J Cardiovasc Electrophysiol 26(2):211–222
Gu WL, Chen CX, Wu Q, Lü J, Liu Y, Zhang SJ (2010) Effects of Chinese herb medicine Radix Scrophulariae on ventricular remodeling. Pharmazie 65:770–775
Guo Y, Wu X, Zheng X, Lu J, Wang S, Huang X (2017) Usefulness of preoperative transforming growth factor-beta to predict new onset atrial fibrillation after surgical ventricular septal myectomy in patients with obstructive hypertrophic cardiomyopathy. Am J Cardiol 120(1):118–123
Heijman J, Voigt N, Nattel S, Dobrev D (2014) Cellular and molecular electrophysiology of atrial fibrillation initiation, maintenance, and progression. Circ Res 114(9):1483–1499
Hsiao FC, Yeh YH, Chen WJ, Chan YH, Kuo CT, Wang CL, Chang CJ, Tsai HY, Tsai FC, Hsu LA (2016) MMP9 Rs3918242 polymorphism affects tachycardia-induced MMP9 expression in cultured atrial-derived myocytes but is not a risk factor for atrial fibrillation among the Taiwanese. Int J Mol Sci 17(4):521
Huxley RR, Lopez FL, MacLehose RF, Eckfeldt JH, Couper D, Leiendecker-Foster C, Hoogeveen RC, Chen LY, Soliman EZ, Agarwal SK, Alonso A (2013) Novel association between plasma matrix metalloproteinase-9 and risk of incident atrial fibrillation in a case-cohort study: the atherosclerosis risk in communities study. PLoS One 8:e59052
Lewkowicz J, Knapp M, Tankiewicz-Kwedlo A, Sawicki R, Kamińska M, Waszkiewicz E, Musiał WJ (2015) MMP-9 in atrial remodeling in patients with atrial fibrillation. Ann Cardiol Angeiol (Paris) 64(4):285–291
Liu W, Chen J, Xu T, Tian W, Li Y, Zhang Z, Li W (2012) Qiliqiangxin improves cardiac function in spontaneously hypertensive rabbits through the inhibition of cardiac chymase. Am J Hypertens 25:250–260
Ma J, Ma S, Ding C (2017) Curcumin reduces cardiac fibrosis by inhibiting myofibroblast differentiation and decreasing transforming growth factor β1 and matrix metalloproteinase 9 / tissue inhibitor of metalloproteinase 1. Chin J Integr Med 23(5):362–369
Mahajan R, Lau DH, Brooks AG et al (2015) Electrophysiological, electroanatomical, and structural remodeling of the atria as consequences of sustained obesity. J Am Coll Cardiol 66(1):1–11
Moe GW, Laurent G, Doumanovskaia L, Konig A, Hu X, Dorian P (2008) Matrix metalloproteinase inhibition attenuates atrial remodeling and vulnerability to atrial fibrillation in a canine model of heart failure. J Card Fail 14:768–776
Mukherjee R, Herron AR, Lowry AS, Stroud RE, Stroud MR, Wharton JM, Ikonomidis JS, Crumbley AJ III, Spinale FG, Gold MR (2006a) Selective induction of matrixmetalloproteinases and tissue inhibitor of metalloproteinases in atrial andventricular myocardium in patients with atrial fibrillation. Am J Cardiol 97:532–537
Nakajima H, Nakajima HO, Salcher O, Dittiè AS, Dembowsky K, Jing S, Field LJ (2000) Atrial but not ventricular fibrosis in mice expressing a mutant transforming growth factor-beta(1) transgene in the heart. Circ Res 86(5):571–579
Nakatani Y, Nishida K, Sakabe M, Kataoka N, Sakamoto T, Yamaguchi Y, Iwamoto J, Mizumaki K, Fujiki A, Inoue H (2013) Tranilast prevents atrial remodeling and development of atrial fibrillation in a canine model of atrial tachycardia and left ventricular dysfunction. J Am Coll Cardiol 61:582–588
Nattel S, Harada M (2014) Atrial remodeling and atrial fibrillation: recent advances and translational perspectives. J Am Coll Cardiol 63:2335–2345
Okumura K (2007) Extracellular matrix remodeling as a cause of persistent atrial fibrillation: another therapeutic target. J Cardiovasc Electrophysiol 18:1083–1085
Pellman J, Lyon RC, Sheikh F (2010a) Extracellular matrix remodeling in atrial fibrosis: mechanisms and implications in atrial fibrillation. J Mol CellCardiol 48:461–467
Schiller M, Javelaud D, Mauviel A (2004) TGF-beta-induced SMAD signaling and gene regulation: consequences for extracel-lular matrix remodeling and wound healing. J Dermatol Sci 35:83–92
Shen S, Jiang H, Bei Y et al (2017) Qiliqiangxin attenuates adverse cardiac remodeling after myocardial infarction in ovariectomized mice via activation of PPARγ. Cell Physiol Biochem 42(3):876–888
Spinale FG (2007) Myocardial matrix remodeling and the matrix metalloproteinases: influence on cardiac form and function. Physiol Rev 87:1285–1342
Takemoto Y, Ramirez RJ, Yokokawa M et al (2016) Galectin-3 regulates atrial fibrillation remodeling and predicts catheter ablation outcomes. JACC Basic Transl Sci 1(3):143–154
Thanigaimani S, Lau DH, Agbaedeng T, Elliott AD, Mahajan R, Sanders P (2017) Molecular mechanisms of atrial fibrosis: implications for the clinic. Expert Rev Cardiovasc Ther 15(4):247–256
Verheule S, Sato T, Everett TIV, Engle SK, Otten D, Rubart-von der Lohe M, Nakajima HO, Nakajima H, Field LJ, Olgin JE (2004) Increased vulnerability to atrial fibrillation in transgenic mice with selective atrial fibrosis caused by overexpression of TGF-beta1. CircRes 94:1458–1465
Wang J, Zhou J, Wang Y et al (2017a) Qiliqiangxin protects against anoxic injury in cardiac microvascular endothelial cells via NRG-1/ErbB-PI3K/Akt/mTOR pathway. J Cell Mol Med 21(9):1905–1914
Wang H, Zhang X, Yu P, Zhou Q, Zhang J, Zhang H, Zhu H, Zhang C, Yao W, Che L, Xu J, Bei Y, Li X (2017b) Traditional Chinese medication Qiliqiangxin protects against cardiac remodeling and dysfunction in spontaneously hypertensive rats. Int J Med Sci 14(5):506–514
Wijffels MC, Kirchhof CJ, Dorland R, Allessie MA (1995) Atrial fibrillation begets atrial fibrillation. A study in awake chronically instrumented goats. Circulation 92:1954–1968
Wu H, Xie J, Li GN, Chen QH, Li R, Zhang XL, Kang LN, Xu B (2015) Possible involvement of TGF-β/periostin in fibrosis of right atrial appendages in patients with atrial fibrillation. Int J Clin Exp Pathol 8(6):6859–6869
Xie J, Chen Y, Hu C, Pan Q, Wang B, Li X, Geng J, Xu B (2017) Premature senescence of cardiac fibroblasts and atrial fibrosis in patients with atrial fibrillation. Oncotarget 8(35):57981–57990
Xu J, Cui G, Esmailian F, Plunkett M, Marelli D, Ardehali A, Odim J, Laks H, Sen L (2004) Atrial extracellular matrix remod-eling and the maintenance of atrial fibrillation. Circulation 109:363–368
Zhang J, Huang M, Shen S, Wu X, Wu X, Lv P, Zhang H, Wang H, Li X (2017) Qiliqiangxin attenuates isoproterenol-induced cardiac remodeling in mice. Am J Transl Res 9(12):5585–5593
Funding
This work was supported by grants from the Harbin High Level Talent Fund (2013SYYRCYJ06) and the National Nature Scientific Foundation of China (No.81700305).
Author information
Authors and Affiliations
Contributions
Hou Tingting, Liu Guangzhong, Zang Yanxiang, and Li Weimin conceived and designed research. Hou TingTing, Liu Guangzhong, Zang Yangxiang, and Sun Li conducted experiments. Liu Guangzhong and Li Weimin contributed new reagents or analytical tools. Hou Tingting and Yu Dongdong analyzed data. Hou Tingting, Liu Guangzhong, and Zang Yanxiang wrote the manuscript. All authors read and approved the manuscript.
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tingting, H., Guangzhong, L., Yanxiang, Z. et al. Qiliqiangxin attenuates atrial structural remodeling in prolonged pacing-induced atrial fibrillation in rabbits. Naunyn-Schmiedeberg's Arch Pharmacol 392, 585–592 (2019). https://doi.org/10.1007/s00210-018-01611-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-018-01611-0