Abstract
Introduction
We set out to determine if insertion of a retropubic tension-free vaginal tape (TVT) sling at the time of pelvic organ prolapse surgery improves continence outcomes in women with pre-operative occult stress incontinence (OSI) or asymptomatic urodynamic stress incontinence (USI).
Methods
We conducted a randomised controlled study of prolapse surgery with or without a TVT midurethral sling. The pre- and post-operative assessment at 6 months included history, physical examination and urodynamic testing. Quality of life (QOL) and treatment success was assessed with the UDI-6 SF, IIQ-7 SF and a numerical success score. The primary outcome was symptomatic stress urinary incontinence (SUI) requiring continence surgery (TVT) at 6 months. Long-term follow-up continued to a minimum of 24 months. Secondary outcomes were quality of life parameters.
Results
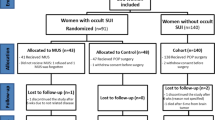
Eighty women received prolapse surgery alone (n = 43) or prolapse surgery with concurrent TVT (n = 37). Six months following prolapse surgery 3 out of 43 (7 %) patients in the no TVT group requested sling surgery compared with 0 out of 37 (0 %) in the TVT group (ARR 7 % [95 %CI: 3 to 19 %], p = 0.11). After 24 months there was one further participant in the no TVT group who received a TVT for treatment of SUI compared with none in the TVT group (4 out of 43, 9.3 % versus 0 out of 37; ARR 9.3 % [95 %CI: −1 to 22 %], p = 0.06). Both groups showed improvement in QOL difference scores for within-group analysis, without difference between groups.
Conclusion
These results support a policy that routine insertion of a sling in women with OSI at the time of prolapse repair is questionable and should be subject to shared decision-making between clinician and patient.


Similar content being viewed by others
References
Gordon D, Groutz A, Wolman I, Lessing JB, David MP (1999) Development of postoperative urinary stress incontinence in clinically continent patients undergoing prophylactic Kelly plication during genitourinary prolapse repair. Neurourol Urodyn 18(3):193–197, discussion 197–198
Richardson DA, Bent AE, Ostergard DR (1983) The effect of uterovaginal prolapse on urethrovesical pressure dynamics. Am J Obstet Gynecol 146(8):901–905
Rosenzweig BA, Pushkin S, Blumenfeld D, Bhatia NN (1992) Prevalence of abnormal urodynamic test results in continent women with severe genitourinary prolapse. Obstet Gynecol 79(4):539–542
Veronikis DK, Nichols DH, Wakamatsu MM (1997) The incidence of low-pressure urethra as a function of prolapse-reducing technique in patients with massive pelvic organ prolapse (maximum descent at all vaginal sites). Am J Obstet Gynecol 177(6):1305–1313, discussion 1313–1314
Chaikin DC, Groutz A, Blaivas JG (2000) Predicting the need for anti-incontinence surgery in continent women undergoing repair of severe urogenital prolapse. J Urol 163(2):531–534
Bump RC, Fantl JA, Hurt WG (1988) The mechanism of urinary continence in women with severe uterovaginal prolapse: results of barrier studies. Obstet Gynecol 72(3 Pt 1):291–295
Borstad E, Rud T (1989) The risk of developing urinary stress-incontinence after vaginal repair in continent women. A clinical and urodynamic follow-up study. Acta Obstet Gynecol Scand 68(6):545–549
Bergman A, Koonings PP, Ballard CA (1988) Predicting postoperative urinary incontinence development in women undergoing operation for genitourinary prolapse. Am J Obstet Gynecol 158(5):1171–1175
Bump RC, Hurt WG, Theofrastous JP et al (1996) Randomized prospective comparison of needle colposuspension versus endopelvic fascia plication for potential stress incontinence prophylaxis in women undergoing vaginal reconstruction for stage III or IV pelvic organ prolapse. Am J Obstet Gynecol 175(2):326–333, discussion 333–335
Haylen BT, de Ridder D, Freeman RM et al (2010) An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J Pelvic Floor Dysfunct 21(1):5–26
Visco AG, Brubaker L, Nygaard I et al (2008) The role of preoperative urodynamic testing in stress-continent women undergoing sacrocolpopexy: the Colpopexy and Urinary Reduction Efforts (CARE) randomized surgical trial. Int Urogynecol J Pelvic Floor Dysfunct 19(5):607–614
Barnes NM, Dmochowski RR, Park R, Nitti VW (2002) Pubovaginal sling and pelvic prolapse repair in women with occult stress urinary incontinence: effect on postoperative emptying and voiding symptoms. Urology 59(6):856–860
Colombo M, Maggioni A, Scalambrino S, Vitobello D, Milani R (1997) Surgery for genitourinary prolapse and stress incontinence: a randomized trial of posterior pubourethral ligament plication and Pereyra suspension. Am J Obstet Gynecol 176(2):337–343
Groutz A, Gordon D, Wolman I et al (2000) The use of prophylactic Stamey bladder neck suspension to prevent post-operative stress urinary incontinence in clinically continent women undergoing genitourinary prolapse repair. Neurourol Urodyn 19(6):671–676
Ulmsten U, Falconer C, Johnson P et al (1998) A multicenter study of tension-free vaginal tape (TVT) for surgical treatment of stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 9(4):210–213
Nilsson CG (1998) The tensionfree vaginal tape procedure (TVT) for treatment of female urinary incontinence. A minimal invasive surgical procedure. Acta Obstet Gynecol Scand Suppl 168:34–37
Ulmsten U, Henriksson L, Johnson P, Varhos G (1996) An ambulatory surgical procedure under local anesthesia for treatment of female urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 7(2):81–85, discussion 85–86
Altman DG (1998) Confidence intervals for the number needed to treat. BMJ 317(7168):1309–1312
Ludbrook J (1998) Multiple comparison procedures updated. Clin Exp Pharmacol Physiol 25(12):1032–1037
Jha S, Moran PA (2007) National survey on the management of prolapse in the UK. Neurourol Urodyn 26(3):325–331, discussion 332
Vanspauwen R, Seman E, Dwyer P (2010) Survey of current management of prolapse in Australia and New Zealand. Aust N Z J Obstet Gynaecol 50(3):262–267
Fatton B (2009) Is there any evidence to advocate SUI prevention in continent women undergoing prolapse repair? An overview. Int Urogynecol J Pelvic Floor Dysfunct 20(2):235–245
Brubaker L, Cundiff GW, Fine P (2006) Abdominal sacrocolpopexy with Burch colposuspension to reduce urinary stress incontinence. N Engl J Med 354(15):1557–1566
Brubaker L, Nygaard I, Richter HE (2008) Two-year outcomes after sacrocolpopexy with and without burch to prevent stress urinary incontinence. Obstet Gynecol 112(1):49–55
Wei JT, Nygaard I, Richter HE et al (2012) A midurethral sling to reduce incontinence after vaginal prolapse repair. N Engl J Med 366(25):2358–2367
Lee JK, Dwyer PL, Rosamilia A, Lim YN, Polyakov A, Stav K (2011) Persistence of urgency and urge urinary incontinence in women with mixed urinary symptoms after midurethral slings: a multivariate analysis. BJOG 118(7):798–805
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schierlitz, L., Dwyer, P.L., Rosamilia, A. et al. Pelvic organ prolapse surgery with and without tension-free vaginal tape in women with occult or asymptomatic urodynamic stress incontinence: a randomised controlled trial. Int Urogynecol J 25, 33–40 (2014). https://doi.org/10.1007/s00192-013-2150-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-013-2150-7