Abstract
Background
Initial non-operative management of children with complicated appendicitis has been well studied but when comparing emergency procedures the long-term effectiveness of interval appendectomy remains undefined. This study aimed to determine the effects of interval appendectomy from the perspective of long-term follow-up.
Methods
A retrospective review of patients with complicated appendicitis between 2010 and 2017 was performed. The medical records of 471 patients with initial non-operative therapy and 377 patients treated with emergency appendectomy who served as controls were reviewed. Propensity score matching was performed to adjust for any potential selection bias in the two strategies. A comparison of the clinical outcomes, including short- and long-term postoperative complications, was conducted in the 348 matched patients.
Results
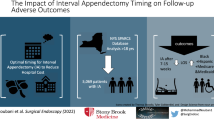
On presentation, there were no differences in age, weight, sex distribution, white blood cell (WBC), or procalcitonin (PCT) between the two groups, except for days of symptoms. The patients undergoing emergency appendectomy had a high American Society of Anesthesiology (ASA) score (p = 0.002). The patients who underwent initial non-operative therapy had a lower complication rate, including surgical wound infection [odds ratio (OR), 3.77; 95% CI 2.59–5.50; p < 0.001) and postoperative peritonitis or abscess (OR, 3.81; 95% CI 1.79–8.12; p < 0.001) than those who underwent emergency appendectomy. Furthermore, the incidence of adhesive small bowel obstruction (ASBO) was lower in patients who underwent initial non-operative therapy than in patients who underwent emergency appendectomy (OR, 4.6; 95% CI 0.99–21.41; p = 0.032).
Conclusions
Initial non-operative therapy with interval appendectomy was feasible for most patients with appendiceal abscesses and had advantages in terms of postoperative complications, especially regarding long-term obstruction events. Therefore, initial non-operative therapy with interval appendectomy should be considered the first treatment of choice for pediatric patients with complicated appendicitis.

Similar content being viewed by others
References
Hanson AL, Crosby RD, Basson MD. Patient preferences for surgery or antibiotics for the treatment of acute appendicitis. JAMA Surg. 2018;153:471–8.
Al-Kurd A, Mizrahi I, Siam B, et al. Outcomes of interval appendectomy in comparison with appendectomy for acute appendicitis. J Surg Res. 2018;225:90–4.
Kaminski A, Liu IL, Applebaum H, et al. Routine interval appendectomy is not justified after initial non-operative treatment of acute appendicitis. Arch Surg. 2005;140:897–901.
Janik JS, Ein SH, Shandling B, Simpson JS, Stephens CA. Nonsurgical management of appendiceal mass in late presenting children. J Pediatr Surg. 1980;15:574–6.
Talishinskiy T, Limberg J, Ginsburg H, et al. Factors associated with failure of nonoperative treatment of complicated appendicitis in children. J Pediatr Surg. 2016;51:1174–6.
Albright JB, Fakhre GP, Nields WW, et al. Incidental appendectomy: 18-year pathologic survey and cost effectiveness in the nonmanaged-care setting. J Am Coll Surg. 2007;205:298–306.
Andersson RE, Petzold MG. Nonsurgical treatment of appendiceal abscess or phlegmon. A systematic review and meta-analysis. Ann Surg 2007;246:741–748.
Cheng Y, Xiong X, Lu J, et al. Early versus delayed appendicectomy for appendiceal phlegmon or abscess. Cochrane Database Syst Rev. 2017;6:11670.
Darwazeh G, Cunningham SC, Kowdley GC. A systematic review of perforated appendicitis and phlegmon: interval appendectomy or wait-and-see? Am Surg. 2016;82:11–5.
Cheng O, Cheng L, Burjonrappa S. Facilitating factors in same-day discharge after pediatric laparoscopic appendectomy. J Surg Res. 2018;229:145–9.
Hajibandeh S, Hajibandeh S, Kelly A, et al. Irrigation versus suction alone in laparoscopic appendectomy: is dilution the solution to pollution? A systematic review and meta-analysis. Surg Innov. 2018;25:174–82.
St Peter SD, Aguayo P, Fraser JD, et al. Initial laparoscopic appendectomy versus initial non-operative management and interval appendectomy for perforated appendicitis with abscess: a prospective, randomized trial. J Pediatr Surg. 2010;45:236–40.
Tsao KJ, St Peter SD, Valusek PA, et al. Adhesive small bowel obstruction after appendectomy in children: comparison between the laparoscopic and open approach. J Pediatr Surg. 2007;42:939–42.
Lugo JZ, Avgerinos DV, Lefkowitz AJ, et al. Can interval appendectomy be justified following conservative treatment of perforated acute appendicitis? J Surg Res. 2010;164:91–4.
Muensterer OJ, Puga Nougues C, Adibe OO, et al. Appendectomy using single-incision pediatric endosurgery for acute and perforated appendicitis. Surg Endosc. 2010;24:3201–4.
Young KA, Neuhaus NM, Fluck M, et al. Outcomes of complicated appendicitis: Is conservative management as smooth as it seems? Am J Surg. 2018;215:586–92.
Tannoury J, Abboud B. Treatment options of inflammatory appendiceal masses in adults. World J Gastroenterol. 2013;19:3942–50.
Puapong D, Lee SL, Haigh PI, et al. Routine interval appendectomy in children is not indicated. J Ped Surg. 2007;42:1500–3.
Ouaïssi M, Gaujoux S, Veyrie N, et al. Post-operative adhesions after digestive surgery: their incidence and prevention: review of the literature. J Visc Surg. 2012;149:e104–e114114.
Cao J, Tao F, Xing H, et al. Laparoscopic procedure is not independently associated with the development of intra-abdominal abscess after appendectomy: a multicenter cohort study with propensity score matching analysis. Surg Laparosc Endosc Percutan Tech. 2017;27:409–14.
Kaminski A, Liu IA, Applebaum H, et al. Routine interval appendectomy is not justified after initial nonoperative treatment of acute appendicitis. Arch Surg. 2005;140:897–901.
Garg CP, Vaidya BB, Chengalath MM. Efficacy of laparoscopy in complicated appendicitis. Int J Surg. 2009;7:250–2.
LaPlant MB, Saltzman DA, Rosen JI, et al. Standardized irrigation technique reduces intraabdominal abscess after appendectomy. J Pediatr Surg. 2018;54:728–32.
Ball CG, Kortbeek JB, Kirkpatrick AW, et al. Laparoscopic appendectomy for complicated appendicitis: an evaluation of postoperative factors. Surg Endosc. 2004;18:969–73.
Keckler SJ, Tsao K, Sharp SW, et al. Resource utilization and outcomes from percutaneous drainage and interval appendectomy for perforated appendicitis with abscess. J Pediatr Surg. 2008;43:977–80.
Author information
Authors and Affiliations
Contributions
YZ, HZ designed and analyzed the data and evaluated the manuscript. QD, BC, LQ performed the statistical calculations and analyzed the data. CG analyzed the data and wrote the paper.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interests.
Rights and permissions
About this article
Cite this article
Zhang, Y., Deng, Q., Zhu, H. et al. Intermediate-term evaluation of interval appendectomy in the pediatric population. Eur J Trauma Emerg Surg 47, 1041–1047 (2021). https://doi.org/10.1007/s00068-019-01277-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-019-01277-0