Abstract
Objective
We tested the hypothesis that deep anesthesia with sevoflurane, known as a potent immunomodulator, for 4 h would worsen the 24-h outcomes of rats through modulation of the inflammatory responses.
Methods
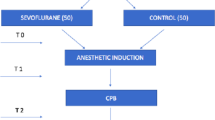
Forty-nine male Wistar rats, administered low dose of lipopolysaccharide (0.5 mg/kg) intravenously to elicit moderate inflammatory responses mimicked mild surgical stress, underwent one minimum alveolar concentration (MAC) or 2 MAC sevoflurane anesthesia for 4 h. The 24-h survival rate, arterial blood gases, plasma interleukin (IL)-6 and tumor necrosis factor (TNF)-α concentrations, and rate of T lymphocyte apoptosis in spleen were evaluated. We further examined the effects of hypotension and TNF-α discharge on the survival rate.
Results
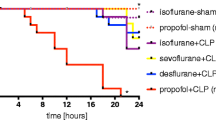
The survival rate in 2 MAC group was significantly lower accompanied with decreased base excess and increased level of cytokines (IL-6, TNF-α) compared to 1 MAC group. The apoptosis rate did not differ between the two groups. Neither norepinephrine infusion to restore hypotension nor administration of anti-TNF-α antibody improved the outcome in the 2 MAC group.
Conclusions
Deep anesthesia with sevoflurane even for a short-term period augments the release of inflammatory cytokines evoked by inflammatory insults like surgical stress, impairs the acid–base balance, and subsequently deteriorates the outcomes.





Similar content being viewed by others
References
Woods GM, Griffiths DM. Reversible inhibition of natural killer cell activity by volatile anaesthetic agents in vitro. Br J Anaesth. 1986;58:535–9.
de Rossi LW, Brueckmann M, Rex S, Barderschneider M, Buhre W, Rossaint R. Xenon and isoflurane differentially modulate lipopolysaccharide-induced activation of the nuclear transcription factor KB and production of tumor necrosis factor-alpha and interleukin-6 in monocytes. Anesth Analg. 2004;98:1007–12.
Matsuoka H, Kurosawa S, Horinouchi T, Kato M, Hashimoto Y. Inhalation anesthetics induce apoptosis in normal peripheral lymphocytes in vitro. Anesthesiology. 2001;95:1467–72.
Plachinta RV, Hayes JK, Cerilli LA, Rich GF. Isoflurane pretreatment inhibits lipopolysaccharide-induced inflammation in rats. Anesthesiology. 2003;98:89–95.
Lee HT, Emala CW, Joo JD, Kim M. Isoflurane improves survival and protects against renal and hepatic injury in murine septic peritonitis. Shock. 2007;27:373–9.
Herrmann IK, Castellon M, Schwartz DE, Hasler M, Urner M, Hu G, et al. Volatile anesthetics improve survival after cecal ligation and puncture. Anesthesiology. 2013;119:901–6.
Lamkanfi M, Moreira LO, Makena P, Spierings DC, Boyd K, Murray PJ, et al. Caspase-7 deficiency protects from endotoxin-induced lymphocyte apoptosis and improves survival. Blood. 2009;113:2742–5.
Monk TG, Weldon BC. Does depth of anesthesia monitoring improve postoperative outcomes? Curr Opin Anaesthesiol. 2011;24:665–9.
Kalkman CJ, Peelen LM, Moons KG. Pick up the pieces: depth of anesthesia and long-term mortality. Anesthesiology. 2011;114:485–7.
Monk TG, Saini V, Weldon BC, Sigl JC. Anesthetic management and one-year mortality after noncardiac surgery. Anesth Analg. 2005;100:4–10.
Leslie K, Myles PS, Forbes A, Chan MT. The effect of bispectral index monitoring on long-term survival in the B-aware trial. Anesth Analg. 2010;110:816–22.
Kertai MD, Pal N, Palanca BJ, Lin N, Searleman SA, Zhang L, et al. B-Unaware Study Group. Association of perioperative risk factors and cumulative duration of low bispectral index with intermediate-term mortality after cardiac surgery in the B-Unaware Trial. Anesthesiology. 2010;112:1116–27.
Altenburg SP, Martins MA, Silva AR, Cordeiro RS, Castro-Faria-Neto HC. LPS-induced blood neutrophilia is inhibited by alpha 1-adrenoceptor antagonists: a role for catecholamines. J Leuko Biol. 1997;61:689–94.
Fan JH, Feng GG, Huang L, Tang GD, Jiang HX, Xu J. Naofen promotes TNF-α-mediated apoptosis of hepatocytes by activating caspase-3 in lipopolysaccharide-treated rats. World J Gastroenterol. 2014;20:4963–71.
Svoboda P, Kantorova I, Ochmann J. Dynamics of interleukin 1, 2, and 6 and tumor necrosis factor alpha in multiple trauma patients. J Trauma. 1994;36:336–40.
Yao YM, Redl H, Bahrami S, Schlag G. The inflammatory basis of trauma/shock associated multiple organ failure. Inflamm Res. 1998;47:201–10.
Loisa P, Rinne T, Laine S, Hurme M, Kaukinen S. Anti-inflammatory cytokine response and the development of multiple organ failure in severe sepsis. Acta Anaesthesiol Scand. 2003;47:319–25.
Laffey JG, Boylan JF, Cheng DC. The systemic inflammatory response to cardiac surgery: implications for the anesthesiologist. Anesthesiology. 2002;97:215–52.
Buttenschoen K, Buttenschoen DC, Berger D, Vasilescu C, Schafheutle S, Goeltenboth B, et al. Endotoxemia and acute-phase proteins in major abdominal surgery. Am J Surg. 2001;181:36–43.
Hofstetter C, Boost KA, Flondor M, Basagan-Mogol E, Betz C, Homann M, et al. Antiinflammatory effects of sevoflurane and mild hypothermia in endotoxemic rats. Acta Anaesthesiol Scand. 2007;51:893–9.
Hayes JK, Havaleshko DM, Plachinta RV, Rich GF. Isoflurane pretreatment supports hemodynamics and leukocyte rolling velocities in rat mesentery during lipopolysaccharide-induced inflammation. Anesth Analg. 2004;98:999–1006.
Crawford MW, Lerman J, Saldivia V, Carmichael FJ. Hemodynamic and organ blood flow responses to halothane and sevoflurane anesthesia during spontaneous ventilation. Anesth Analg. 1992;75:1000–6.
Gare M, Schwabe DA, Hettrick DA, Kersten JR, Warltier DC, Pagel PS. Desflurane, sevoflurane, and isoflurane affect left atrial active and passive mechanical properties and impair left atrial-left ventricular coupling in vivo: analysis using pressure-volume relations. Anesthesiology. 2001;95:689–98.
Li Y, Cui X, Su J, Haley M, Macarthur H, Sherer K, et al. Norepinephrine increases blood pressure but not survival with anthrax lethal toxin in rats. Crit Care Med. 2009;37:1348–54.
Kalinichenko VV, Mokyr MB, Graf LH Jr, Cohen RL, Chambers DA. Norepinephrine-mediated inhibition of anti-tumor cytotoxic T lymphocyte generation involves a beta-adrenergic receptor mechanism and decreased TNF-alpha gene expression. J Immunol. 1999;163:2492–9.
Hofstetter C, Boost KA, Hoegl S, Flondor M, Scheller B, Muhl H, et al. Norepinephrine and vasopressin counteract anti-inflammatory effects of isoflurane in endotoxemic rats. Int J Mol Med. 2007;20:597–604.
Hotchkiss RS, Chang KC, Swanson PE, Tinsley KW, Hui JJ, Klender P, et al. Caspase inhibitors improve survival in sepsis: a critical role of the lymphocyte. Nat Immunol. 2000;1:496–501.
Schwulst SJ, Muenzer JT, Peck-Palmer OM, Chang KC, Davis CG, McDonough JS, et al. Bim siRNA decreases lymphocyte apoptosis and improves survival in sepsis. Shock. 2008;30:127–34.
Kotani N, Hashimoto H, Sessler DI, Yasuda T, Ebina T, Muraoka M, et al. Expression of genes for proinflammatory cytokines in alveolar macrophages during propofol and isoflurane anesthesia. Anesth Analg. 1999;89:1250–6.
Morisaki H, Suematsu M, Wakabayashi Y, Moro-oka S, Fukushima K, Ishimura Y, et al. Leukocyte-endothelium interaction in the rat mesenteric microcirculation during halothane or sevoflurane anesthesia. Anesthesiology. 1997;87:591–8.
Newham P, Ross D, Ceuppens P, Das S, Yates JW, Betts C, et al. Determination of the safety and efficacy of therapeutic neutralization of tumor necrosis factor-α (TNF-α) using AZD9773, an anti-TNF-α immune Fab, in murine CLP sepsis. Inflamm Res. 2014;63:149–60.
Kidani Y, Taniguchi T, Kanakura H, Takemoto Y, Tsuda K, Yamamoto K. Sevoflurane pretreatment inhibits endotoxin-induced shock in rats. Anesth Analg. 2005;101:1152–6.
Held HD, Boettcher S, Hamann L, Uhlig S. Ventilation-induced chemokine and cytokine release is associated with activation of nuclear factor- κB and is blocked by steroids. Am J Respir Crit Care Med. 2001;163:711–6.
Tremblay L, Valenza F, Ribeiro SP, Li J, Slutsky AS. Injurious ventilatory strategies increase cytokines and c-fos m-RNA expression in an isolated rat lung model. J Clin Invest. 1997;99:944–52.
Altemeier WA, Matute-Bello G, Frevert CW, Kawata Y, Kajikawa O, Martin TR, et al. Mechanical ventilation with moderate tidal volumes synergistically increases lung cytokine response to systemic endotoxin. Am J Physiol Lung Cell Mol Physiol. 2004;287:L533–42.
Acknowledgments
All authors gratefully thank Dr. Katsuya Mori for his excellent advice to perform the present study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Additional information
Responsible Editor: Ji Zhang.
Rights and permissions
About this article
Cite this article
Inoue, K., Suzuki, T., Igarashi, T. et al. Deep anesthesia worsens outcome of rats with inflammatory responses. Inflamm. Res. 65, 563–571 (2016). https://doi.org/10.1007/s00011-016-0940-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-016-0940-3