Abstract
Purpose
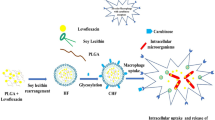
The purpose of this study is to know the effect of uptake of mycobacteria on the phagocytic activity of alveolar macrophage (Mφ) cells toward poly(lactic-co-glycolic) acid (PLGA) microspheres (MS) loaded with the anti-tuberculosis agent rifampicin (RFP-PLGA MS).
Materials and Methods
Biological functions such as phagocytic activity toward PLGA MS loaded with fluorescent coumarin (cPLGA MS) and toward polystyrene latex MS (PSL MS), and generation of tumor necrosis factor-α (TNF-α) and nitric oxide (NO) were examined using alveolar Mφ cell NR8383 after they had phagocytosed Mycobacterium bovis Calmette-Guérin (BCG), heat-killed BCG (h-kBCG) or Escherichia coli.
Results
The ingestion of BCG, h-kBCG, and E. coli did not affect the viability of the Mφ cells within 2 days. The phagocytosis caused generation of TNF-α and NO, being more significant with E. coli than with both types of BCGs. The phagocytosis of both types of BCGs stimulated the phagocytic uptake of cPLGA and PSL MS’s, which took place prior to the generation of TNF-α or NO, but that of E. coli suppressed the uptake of both MS’s.
Conclusion
Mycobacterial infection stimulated the phagocytic uptake toward cPLGA MS. These results suggest that RFP-PLGA MS is favorable for overcoming tuberculosis.










Similar content being viewed by others
Abbreviations
- BCG:
-
Mycobacterium bovis Calmette-Guérin
- h-kBCG:
-
heat-killed BCG
- CFU:
-
colony-forming units
- ELISA:
-
enzyme-linked immunosorbent assay
- FBS:
-
fetal bovine serum
- Mφ:
-
macrophage
- MOI:
-
multiplicity of infection
- MTB:
-
Mycobacterium tuberculosis
- MS:
-
microspheres
- NO:
-
nitric oxide
- PBS:
-
phosphate-buffered saline
- PLGA:
-
poly(lactic-co-glycolic) acid
- cPLGA MS:
-
PLGA MS loaded with coumarin 6
- RFP-PLGA MS:
-
PLGA MS loaded with rifampicin
- PSL MS:
-
polystyrene latex MS
- RFP:
-
rifampicin
- TNF-α:
-
tumor necrosis factor-α
- WST-8:
-
2-(2-methoxy-4-nitrophenyl)-3-(4-nitrophenyl)-5-(2,4-disulfophenyl)-2H-tetrazolium, monosodium salt
References
D. H. Bowden. The alveolar macrophage. Environ. Health Perspect. 55:327–341 (1984).
S. Mukherjee, R. N. Ghosh, and F. R. Maxfield. Endocytosis. Physiol. Rev. 77:759–803 (1997).
G. Ferrari, H. Langen, M. Naito, and J. Pieters. A coat protein on phagosomes involved in the intracellular survival of mycobacteria. Cell 97:435–447 (1999).
S. Sturgill-Koszycki, P. H. Schlesinger, P. Chakraborty, P. L. Haddix, H. L. Collins, A. K. Fok, R. D. Allen, S. L. Gluck, J. Heuser, and D. G. Russell. Lack of acidification in Mycobacterium phagosomes produced by exclusion of the vesicular proton-ATPase. Science 263:678–681 (1994).
K. Makino, T. Nakajima, M. Shikamura, F. Ito, S. Ando, C. Kochi, H. Inagawa, G. Soma, and H. Terada. Efficient intracellular delivery of rifampicin to alveolar macrophages using rifampicin-loaded PLGA microspheres: effects of molecular weight and composition of PLGA on release of rifampicin. Colloids Surf. B 36:35–42 (2004).
A. Yoshida, M. Matumoto, H. Hshizume, Y. Oba, T. Tomishige, H. Inagawa, C. Kohchi, M. Hino, F. Ito, K. Tomoda, T. Nakajima, K. Makino, H. Terada, and G. Soma. Selective delivery of rifampicin incorporated into poly(DL-lactic-co-glycolic) acid microspheres after phagocytotic uptake by alveolar macrophages, and the killing effect against intracellular Mycobacterium bovis Calmette-Guérin. Microbes. Infect. 8:2484–2491 (2006).
R. Sharma, P. Muttil, A. B. Yadav, S. K. Rath, V. K. Bajpai, U. Mani, and A. Misra. Uptake of inhalable microparticles affects defense responses of macrophages infected with Mycobacterium tuberculosis H37Ra. J. Antimicrob. Chemother. 59:499–506 (2007).
Z. Xing, A. Zganiacz, and M. Santosuosso. Role of IL-12 in macrophage activation during intracellular infection: IL-12 and mycobacteria synergistically release TNF-α and nitric oxide from macrophages via IFN-γ induction. J. Leukoc. Biol. 68:897–902 (2000).
C. H. Wang and H. P. Kuo. Nitric oxide modulates interleukin-1β and tumour necrosis factor-α synthesis, and disease regression by alveolar macrophages in pulmonary tuberculosis. Respirology 6:79–84 (2001).
J. L. Flynn, M. M. Goldstein, J. Chan, K. J. Triebold, K. Pfeffer, C. J. Lowenstein, R. Schrelber, T. W. Mak, and B. R. Bloom. Tumor necrosis factor-α is required in the protective immune response against Mycobacterium tuberculosis in mice. Immunity 2:561–572 (1995).
S. E. Valone, E. A. Rich, R. S. Wallis, and J. J. Ellener. Expression of tumor necrosis factor in vitro by human mononuclear phagocytes stimulated with whole Mycobacterium bovis BCG and mycobacterial antigens. Infect. Immun. 56:3313–3315 (1988).
A. Aderem. Phagocytosis and the inflammatory response. J. Infect. Dis. 187(Suppl 2):S340–S345 (2003).
P. Henneke, O. Takeuchi, R. Malley, E. Lien, R. R. Ingalls, M. W. Freeman, T. Mayadas, V. Nizet, S. Akira, D. L. Kasper, and D. T. Golenbock. Cellular activation, phagocytosis, and bactericidal activity against group B streptococcus involve parallel myeloid differentiation factor 88-dependent and independent signaling pathways. J. Immunol. 169:3970–3977 (2002).
B. J. van Lenten and A. M. Fogelman. Lipopolysaccharide-induced inhibition of scavenger receptor expression in human monocyte-macrophages is mediated through tumor necrosis factor-α. J. Immunol. 148:112–116 (1992).
J. E. Albina, S. Cui, R. B. Mateo, and J. S. Reichner. Nitric oxide-mediated apoptosis in murine peritoneal macrophages. J. Immunol. 150:5080–5085 (1993).
S. Akira, K. Takeda, and T. Kaisho. Toll-like receptors: critical proteins linking innate and acquired immunity. Nat. Immunol. 2:675–680 (2001).
J. Panyam, W. Zhou, S. Prabha, S. K. Sahoo, and V. Labhasetwar. Rapid endo-lysosomal escape of poly(DL-lactide-co-glycolide) nanoparticles: implications for drug and gene delivery. FASEB J. 16:1217–1226 (2002).
K. Tomoda, S. Kojima, M. Kajimoto, D. Watanabe, T. Nakajima, and K. Makino. Effects of pulmonary surfactant system on rifampicin release from rifampicin-loaded PLGA microspheres. Colloids Surf. B 45:1–6 (2005).
T. Hasegawa, K. Hirota, K. Tomoda, F. Ito, H. Inagawa, C. Kochi, G. Soma, K. Makino, and H. Terada. Phagocytic activity of alveolar macrophages toward polystyrene latex microspheres and PLGA microspheres loaded with anti-tuberculosis agent. Colloids Surf. B 60:221–228 (2007).
T. Hasegawa, K. Iijima, K. Hirota, T. Nakajima, K. Makino, and H. Terada. Exact determination of phagocytic activity of alveolar macrophages toward polymer microspheres by elimination of those attached to the macrophage membrane. Colloids Surf. B (in press).
H. Tominaga, M. Ishiyama, F. Ohseto, K. Sasamoto, T. Hamamoto, K. Suzuki, and M. Watanabe. A water-soluble tetrazolium salt useful for colorimetric cell viability assay. Anal. Commun. 36:47–50 (1999).
B. G. Jones, P. A. Dickinson, M. Gumbleton, and I. W. Kellaway. The inhibition of phagocytosis of respirable microspheres by alveolar and peritoneal macrophages. Int. J. Pharm. 236:65–79 (2002).
S. Ben-Efraim and T. Diamantstein. Mitogenic and adjuvant activity of a methanol extraction residue (MER) of tubercle bacilli on mouse lymphoid cells in vitro. Immunol. Commun. 4:565–577 (1975).
I. Azuma, T. Taniyama, K. Sugimura, A. A. Aladin, and Y. Yamamura. Mitogenic activity of the cell walls of mycobacteria, nocardia, corynebacteria and anaerobic coryneforms. Jpn. J. Microbiol. 20:263–271 (1976).
A. P. Gobert, S. Semballa, S. Daulouede, S. Lesthelle, M. Taxile, B. Veyret, and P. Vincendeau. Murine macrophages use oxygen- and nitric oxide-dependent mechanisms to synthesize S-nitroso-albumin and to kill extracellular trypanosomes. Infect. Immun. 66:4068–4072 (1998).
G. S. Timmins, S. Master, F. Rusnak, and V. Deretic. Requirements for nitric oxide generation from isoniazid activation in vitro and inhibition of mycobacterial respiration in vivo. J. Bacteriol. 186:5427–5431 (2004).
J. S. Beckman, T. W. Beckman, J. Chen, P. A. Marshall, and B. A. Freeman. Apparent hydroxyl radical production by peroxynitrite: Implications for endothelial injury from nitric oxide and superoxide. Proc. Natl. Acad. Sci. U. S. A. 87:1620–1624 (1990).
K. Hirota, T. Hasegawa, H. Hinata, F. Ito, H. Inagawa, C. Kochi, G. Soma, K. Makino, and H. Terada. Optimum conditions for efficient phagocytosis of rifampicin-loaded PLGA microspheres by alveolar macrophages. J. Control. Release 119:69–76 (2007).
Y. Tabata and Y. Ikada. Phagocytosis of polymer microspheres by macrophages. In Advances in Polymer Science, vol. 94. Springer, Berlin, 1990, pp. 107–141.
H. Kawaguchi, N. Koiwai, Y. Ohtsuka, M. Miyamoto, and S. Sasakawa. Phagocytosis of latex particles by leucocytes. I. Dependence of phagocytosis on the size and surface potential of particles. Biomaterials 7:61–66 (1986).
A. Zhang, M. J. Groves, and M. E. Klegerman. The surface charge of cells of Mycobacterium bovis BCG vaccine, TiceTm substrain. Microbios. 53:191–195 (1988).
J. Chen and B. Koopman. Effect of fluorochromes on bacterial surface properties and interaction with granular media. Appl. Environ. Microbiol. 63:3941–3945 (1997).
H. Häcker, C. Fürmann, H. Wagner, and G. Häcker. Caspase-9/-3 activation and apoptosis are induced in mouse macrophages upon ingestion and digestion of Escherichia coli bacteria. J. Immunol. 169:3172–3179 (2002).
M. Rojas, L. F. Barrera, G. Puzo, and L. F. Garcia. Differential induction of apoptosis by virulent Mycobacterium tuberculosis in resistant and susceptible murine macrophages: role of nitric oxide and mycobacterial products. J. Immunol. 159:1352–1361 (1997).
J. Lee, H. G. Remold, M. H. Ieong, and H. Kornfeld. Macrophage apoptosis in response to high intracellular burden of Mycobacterium tuberculosis is mediated by a novel caspase-independent pathway. J. Immunol. 176:4267–4274 (2006).
T. Kaisho and S. Akira. Toll-like receptor function and signaling. J. Allergy. Clin. Immunol. 117:979–987 (2006).
E. Rhoades, F-. F. Hsu, J. B. Torrelles, J. Turk, D. Chatterjee, and D. G. Russel. Identification and macrophage-activating activity of glycolipids released from intracellular Mycobacterium bovis BCG. Mol. Microbiol. 48:875–888 (2003).
M. J. Lyons, T. Yoshimura, and D. N. McMurray. Mycobacterium bovis BCG vaccination augments interleukin-8 mRNA expression and protein production in guinea pig alveolar macrophages infected with Mycobacterium tuberculosis. Infect. Immun. 70:5471–5478 (2002).
S. Saito and M. Nakano. Nitric oxide production by peritoneal macrophages of Mycobacterium bovis BCG-infected or non-infected mice: regulatory roles of T lymphocytes and cytokines. J. Leukoc. Biol. 59:908–915 (1996).
J. A. Hamerman and A. Aderem. Functional transitions in macrophages during in vivo infection with Mycobacterium bovis Bacillus Calmette-Guérin. J. Immunol. 167:2227–2233 (2001).
M. J. Fenton, M. W. Vermeulen, S. Kim, M. Burdick, R. M. Strieter, and H. Kornfeld. Induction of gamma interferon production in human alveolar macrophages by Mycobacterium tuberculosis. Infect. Immun. 65:5149–5156 (1997).
K. D. Srivastava, W. N. Rom, J. Jagirdar, T. Yie, T. Gordon, and K. Tchou-Wong. Crucial role of interleukin-1β and nitric oxide synthase in silica-induced inflammation and apoptosis in mice. Am. J. Respir. Crit. Care Med. 165:527–533 (2002).
T. Gotoh and M. Mori. Arginase II downregulates nitric oxide (NO) production and prevents NO-mediated apoptosis in murine macrophage-derived RAW 264.7 cells. J. Cell Biol. 144:427–434 (1999).
M. A. Chambers, B. G. Marshall, A. Wangoo, A. Bune, H. T. Cook, R. J. Shaw, and D. B. Young. Differential responses to challenge with live and dead Mycobacterium bovis Bacillus Calmette-Guérin. J. Immunol. 158:1742–1748 (1997).
E. B. Lasunskaia, M. N. N. Campos, M. R. M. de Andrade, R. A. Damatta, T. L. Kipnis, M. Einicker-Lamas, and W. D. Da Silva. Mycobacteria directly induce cytoskeletal rearrangements for macrophage spreading and polarization through TLR2-dependent PI3K signaling. J. Leukoc. Biol. 80:1480–1490 (2006).
R. Haworth, N. Platt, S. Keshav, D. Hughes, E. Darley, H. Suzuki, Y. Kurihara, T. Kodama, and S. Gordon. The macrophage scavenger receptor type A is expressed by activated macrophages and protects the host against lethal endotoxic shock. J. Exp. Med. 186:1431–1439 (1997).
T. Doi, K. Higashino, Y. Kurihara, Y. Wada, T. Miyazaki, H. Nakamura, S. Uesugi, T. Imanishi, Y. Kawabe, H. Itakura, Y. Yazaki, A. Matsumoto, and T. Kodama. Charged collagen structure mediates the recognition of negatively charged macromolecules by macrophage scavenger receptors. J. Biol. Chem. 268:2126–2133 (1993).
S. Józefowski, M. Arredouani, T. Sulahian, and L. Kobzik. Disparate regulation and function of the class A scavenger receptors SR-AI/II and MARCO. J. Immunol. 175:8032–8041 (2005).
K. Makino, N. Yamamoto, K. Higuchi, N. Harada, H. Ohshima, and H. Terada. Phagocytic uptake of polystyrene microspheres by alveolar macrophages: effects of the size and surface properties of the microspheres. Colloids Surf. B 27:33–39 (2003).
Acknowledgements
This study was supported, in part, by the “High-Tech Research Center” Project for Private Universities with a matching fund subsidy from MEXT (Ministry for Education, Culture, Sports, Science, and Technology) of Japan, 2004–2008, and by a grant-in-aid for scientific research from MEXT (No. 15300170 to H.T.).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hirota, K., Tomoda, K., Inagawa, H. et al. Stimulation of Phagocytic Activity of Alveolar Macrophages Toward Artificial Microspheres by Infection with Mycobacteria. Pharm Res 25, 1420–1430 (2008). https://doi.org/10.1007/s11095-007-9525-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-007-9525-8