Summary
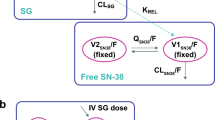
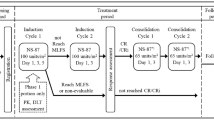
This study was designed to determine the safety and optimal dosing of TAS-102, a novel oral combination of ααα-trifluorothymidine (FTD) and an inhibitor of thymidine phoshorylase, in patients with solid tumors. Patients who met the eligibility criteria were treated with one of two different TAS-102 regimens: once per day on either days 1–5 and 8–12 every 4 weeks (schedule A) or days 1–5 every 3 weeks (schedule B). The primary objectives were the determination of the maximum tolerated dose, dose-limiting toxicities (DLTs), and recommended phase II dose. Pharmacokinetic analysis was conducted during courses 1 and 2. Sixty-three patients received a total of 172 courses of therapy with the median number of courses delivered on both schedules being 2. DLTs were observed in three patients on schedule A, 70 mg/m2/day (1) and 110 mg/m2/day (2); and in five patients on schedule B, 120 mg/m2/day (1), 170 mg/m2/day (2), 180 mg/m2/day (2). Granulocytopenia was the DLT in seven of the eight cases. The most frequent toxicities were nausea, fatigue, granulocytopenia, anemia, diarrhea, and abdominal pain. Twelve patients, 6 on schedule A and 6 on schedule B, were treated at the recommended phase II dose, with good tolerance. No objective responses were seen in this heavily pretreated, 5-FU-refractory population. The pharmacokinetic parameters of FTD are a T max of 0.53 to 3.15 h, t 1/2 of 1.46 to 4.20 h, volume of distribution of 0.0526 to 0.483 l/kg, and clearance of 0.0194 to 0.197 1/h/kg. The recommended phase II doses for TAS-102 are 100 mg/m2/day on schedule A and 160 mg/m2/day on schedule B. Future development of TAS-102 should focus upon multiple daily dosing schedules.

Similar content being viewed by others
References
No authors listed (1992) Modulation of fluorouracil by leucovorin in patients with advanced colorectal cancer: evidence in terms of response rate. Advanced Colorectal Cancer Meta-Analysis Project. J Clin Oncol 10(6):896–903
Miwa M et al (1998) Design of a novel oral fluoropyrimidine carbamate, capecitabine, which generates 5-fluorouracil selectively in tumours by enzymes concentrated in human liver and cancer tissue. Eur J Cancer 34(8):1274–1281
Schuller J et al (2000) Preferential activation of capecitabine in tumor following oral administration to colorectal cancer patients. Cancer Chemother Pharmacol 45(4):291–297
Longley DB, Harkin DP, Johnston PG (2003) 5-fluorouracil: mechanisms of action and clinical strategies. Nat Rev Cancer 3(5):330–338
Emura T et al (2004) A novel antimetabolite, TAS-102 retains its effect on FU-related resistant cancer cells. Int J Mol Med 13(4):545–549
Temmink OH et al (2005) Determinants of trifluorothymidine sensitivity and metabolism in colon and lung cancer cells. Anticancer Drugs 16(3):285–292
Ansfield FJ, Ramirez G (1971) Phase I and II studies of 2¢-deoxy-5-(trifluoromethyl)-uridine (NSC-75520). Cancer Chemother Rep 55(2):205–208
Heidelberger C, Dexter DL, Wolberg WH (1970) Clinical pharmacology of 5-trifluoromethyl-2-deoxyuridine (F3TDR). Proc Am Assoc Cancer Res 35
Emura T et al (2005) Potentiation of the antitumor activity of alpha, alpha, alpha-trifluorothymidine by the co-administration of an inhibitor of thymidine phosphorylase at a suitable molar ratio in vivo. Int J Oncol 27(2):449–455
Temmink OH et al (2007) Therapeutic potential of the dual-targeted TAS-102 formulation in the treatment of gastrointestinal malignancies. Cancer Sci 98(6):779–789
Ciccolini J, Evrard A, Cuq P (2004) Thymidine phosphorylase and fluoropyrimidines efficacy: a Jekyll and Hyde story. Curr Med Chem Anticancer Agents 4(2):71–81
Emura T et al (2004) Thymidine kinase and thymidine phosphorylase level as the main predictive parameter for sensitivity to TAS-102 in a mouse model. Oncol Rep 11(2):381–387
Emura T et al (2004) A novel combination antimetabolite, TAS-102, exhibits antitumor activity in FU-resistant human cancer cells through a mechanism involving FTD incorporation in DNA. Int J Oncol 25(3):571–578
Hong DS et al (2006) Phase I study to determine the safety and pharmacokinetics of oral administration of TAS-102 in patients with solid tumors. Cancer 107(6):1383–1390
Sadahiro S et al (2001) A pharmacological study of the weekday-on/weekend-off oral UFT schedule in colorectal cancer patients. Cancer Chemother Pharmacol 47(5):457–460
Sadahiro S et al (1998) Preliminary study on the optimal dosage schedule for oral Tegafur/Uracil (UFT) chemotherapy. International Journal of Clinical Oncology 3:7–12
Miller AB et al (1981) Reporting results of cancer treatment. Cancer 47(1):207–214
Green MC, P.L., Theriault RL et al. (2006) Phase I study to determine the safety of oral administration of TAS-102 on a twice daily (BID) schedule for five days a week (wk) followed by two days rest for two wks, every (Q) four wks in patients (pts) with metastatic breast cancer (MBC). 2006 ASCO Annual Meeting Proceedings Part I. J Clin Oncol 24(18S):10576 (June 20 Supplement)
Wolff RA, H.P., Mita A, et al. (2006) A phase I trial of TAS-102 administered on a three times a day schedule in patients with solid tumors. 2006 ASCO Annual Meeting Proceedings Part I. J Clin Oncol 24(18S):2053 (June 20 Supplement)
Temmink OH et al (2006) Low folate conditions may enhance the interaction of trifluorothymidine with antifolates in colon cancer cells. Cancer Chemother Pharmacol 57(2):171–179
Emura T et al (2004) An optimal dosing schedule for a novel combination antimetabolite, TAS-102, based on its intracellular metabolism and its incorporation into DNA. Int J Mol Med 13(2):249–255
Acknowledgments
Financial support for this research was provided by Taiho Pharmaceuticals. A partial presentation of this material was given at the 2001 American Society of Clinical Oncology meeting, abstract no. 386, and the 2002 American Association of Cancer Research meeting, abstract no. 2754
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Overman, M.J., Varadhachary, G., Kopetz, S. et al. Phase 1 study of TAS-102 administered once daily on a 5-day-per-week schedule in patients with solid tumors. Invest New Drugs 26, 445–454 (2008). https://doi.org/10.1007/s10637-008-9142-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10637-008-9142-3