Abstract
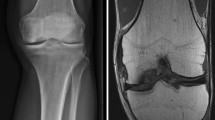
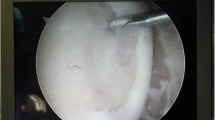
Introduction: The osteochondral transplantation (OCT) is a well accepted treatment option for focal cartilage lesions in the knee joint, whereas the fate of the transplanted cartilage is still unclear and the clinical outcome is variable. The purpose of this study was to evaluate the histological character of autologous transplanted cartilage and to correlate technical aspects and the patients’ history with the clinical outcome. Material and Methods: The OCT was performed in 27 patients (median age of 32 (22–43) years) with a focal chondral lesion at the medial femoral condyle. We investigated the clinical outcome after a median follow-up of 13.5 (5–28) months using the Lysholm-score and the integration of the transplanted plugs using an MRI-scoring system. Biopsy specimens from representative patients (n=8) were evaluated with histological staining and immunohistochemistry. Results: The median Lysholm-score was 80 (range 45–98). The wide range of the Lysholm-score in clinical outcome did not show significant differences in: follow-up, concomitant injuries, defect size or genesis. The MRI analysis revealed in all cases a regular osseous integration of the subchondral bone, but a failed chondral integration. The congruency of the plugs to the joint surface was often incorrect, however a correlation between the MRI-score and the clinical outcome could not be shown. Histology of the transplanted cartilage revealed small changes in immunohistochemistry after a relatively short-term follow-up, whereas the cartilage has still the typical hyaline character. Often, the surrounding cartilage consists of fibrous and granulation tissue. Conclusion: The congruency of the joint surface can not be restored to the original status, particularly in larger defects with irregular shapes. However, we did not find any aspects which affected the function of the knee joint following OCT. It can be assumed that remaining lesions at the surrounding cartilage could maintain the inflammatory process and therefore maintain the pain and a low knee function. Further investigations are needed to specify the effects of the OCT on the transplanted cartilage and its influence on the later clinical outcome.






Similar content being viewed by others
References
Agneskirchner J, Brucker P, Burkart A, Imhoff A (2002) Large osteochondral defects of the femoral condyle: press-fit transplantation of the posterior femoral condyle (MEGA-OATS). Knee Surg Sports Traumatol Arthrosc 10:160–168
Anderson A, Richards D, Pagnani M, Hovis W (1997) Antegrade drilling for osteochondritis dissecans of the knee. Arthroscopy 13:319–324
Aubin PP, Cheah HK, Davis AM, Gross AE (2001) Long-term followup of fresh femoral osteochondral allografts for posttraumatic knee defects. Clin Orthop: S318–S327
Beaver RJ, Mahomed M, Backstein D, Davis A, Zukor DJ, Gross AE (1992) Fresh osteochondral allografts for post-traumatic defects in the knee. A survivorship analysis. J Bone Joint Surg Br 74:105–110
Bobic V (1996) Arthroscopic osteochondral autograft transplantation in anterior cruciate ligament reconstruction: a preliminary clinical study. Knee Surg Sports Traumatol Arthrosc 3:262–264
Buckwalter JA (2002) Articular cartilage injuries. Clin Orthop: 21–37
Czitrom A, Keating S, Gross A (1990) The viability of articular cartilage in fresh osteochondral allografts after clinical transplantation. J Bone Joint Surg [Am] 72:574–81
Garrett JC (1986) Treatment of osteochondral defects of the distal femur with fresh osteochondral allografts: a preliminary report. Arthroscopy 2:222–226
Goymann V (1999) Abrasionschondroplastik. Orthopäde 28:11–18
Grigolo B, Roseti L, De Franceschi L, Piacentini A, Cattini L, Manfredini M, Faccini R, Facchini A (2005) Molecular and immunohistological characterization of human cartilage two years following autologous cell transplantation. J Bone Joint Surg Am 87-A:46–57
Hangody L, Karpati Z, Szerb I, Eberhart R (1996) Autologous osteochondral mosaic.like graft technique for replacing weight bearing cartilage defects. Abstract, 7th Congress of the ESSKA, Budapest, Hungary
Hangody L, Kish G, Karpati Z, Szerb I, Udvarhelyi I (1997) Arthroscopic autogenous osteochondral mosaicplasty for the treatment of femoral condylar articular defects. A preliminary report. Knee Surg Sports Traumatol Arthrosc 5:262–267
Hangody L, Feczko P, Bartha L, Bodo G, Kish G (2001) Mosaicplasty for the treatment of articular defects of the knee and ankle. Clin Orthop: S328–S336
Hangody L, Kish G, Modis L, Szerb I, Gaspar L, Dioszegi Z, Kendik Z (2001) Mosaicplasty for the treatment of osteochondritis dissecans of the talus: two to seven year results in 36 patients. Foot Ankle Int 22:552–558
Hangody L, Fules P (2003) Autologous osteochondral mosaicplasty for the treatment of full-thickness defects of weight-bearing joints: ten years of experimental and clinical experience. J Bone Joint Surg Am 85-A:25–32
Hangody L, Rathonyi GK, Duska Z, Vasarhelyi G, Fules P, Modis L (2004) Autologous osteochondral mosaicplasty. Surgical technique. J Bone Joint Surg Am 86-A:65–72
Herber S, Runkel M, Pitton MB, Kalden P, Thelen M, Kreitner KF (2003) [Indirect MR-arthrography in the follow up of autologous osteochondral transplantation]. Rofo Fortschr Geb Rontgenstr Neuen Bildgeb Verfahr 175:226–233
Hesse W, Hesse I (1979) [Cartilage transplantation in the knee joint experiment—clinic—technique (author’s transl)]. Zentralbl Chir 104:1269–1279
Horas U, Schnettler R, Pelinkovic D, Herr G, Aigner T (2000) [Osteochondral transplantation versus autogenous chondrocyte transplantation. A prospective comparative clinical study]. Chirurg 71:1090–1097
Horas U, Pelinkovic D, Herr G, Aigner T, Schnettler R (2003) Autologous chondrocyte implantation and osteochondral cylinder transplantation in cartilage repair of the knee joint. A prospective, comparative trial. J Bone Joint Surg Am 85-A:185–192
Hunter W (1743) On the structure and deseases of articulating cartilages. Philos Trans R Soc Lond 19:236
Imhoff A, Öttl G, Burkart A, Traub S (1999) Autologous osteochondral transplantation on various joints. Orthopäde 28:33–44
Imhoff AB, Oettl GM (2000) Arthroscopic and Open Techniques for Transplantation of Osteochondral Autografts and Allografts in Various Joints. Surg Technol Int VIII: 249–252
Jakob RP, Franz T, Gautier E, Mainil-Varlet P (2002) Autologous osteochondral grafting in the knee: indication, results, and reflections. Clin Orthop: 170–84
Krueger JA, Thisse P, Ewers BJ, Dvoracek-Driksna D, Orth MW, Haut RC (2003) The extent and distribution of cell death and matrix damage in impacted chondral explants varies with the presence of underlying bone. J Biomech Eng 125:114–119
Lane JG, Tontz WL Jr, Ball ST, Massie JB, Chen AC, Bae WC, Amiel ME, Sah RL, Amiel D (2001) A morphologic, biochemical, and biomechanical assessment of short-term effects of osteochondral autograft plug transfer in an animal model. Arthroscopy 17: 856–863
Laprell H, Petersen W (2001) Autologous osteochondral transplantation using the diamond bone-cuttin system (DBCS): 6–12 years’ follow up of 35 patients with osteochondral defects at the knee joint. Arch Orthop Trauma Surg 121:248–253
Laprell H, Petersen W (2001) Autologous osteochondral transplantation using the diamond bone-cutting system (DBCS): 6–12 years’ follow-up of 35 patients with osteochondral defects at the knee joint. Arch Orthop Trauma Surg 121:248–53
Lysholm J, Gillquist J (1982) Evaluation of knee ligament surgery results with special emphasis on use of scoring scale. Am J Sports Med 10:150–154
Makino T, Fujioka H, Kurosaka M, Matsui N, Yoshihara H, Tsunoda M, Mizuno K (2001) Histologic analysis of the implanted cartilage in an exact-fit osteochondral transplantation model. Arthroscopy 17:747–751
Matsusue Y, Yamamuro T, Hama H (1993) Arthroscopic multiple osteochondral transplantation to the chondral defect in the knee associated with anterior cruciate ligament disruption. Arthroscopy 9:318–321
Meyers MH, Jones RE, Bucholz RW, Wenger DR (1983) Fresh autogenous grafts and osteochondral allografts for the treatment of segmental collapse in osteonecrosis of the hip. Clin Orthop: 107–12
Nabavi-Tabrizi A, Turnbull A, Dao Q, Appleyard R (2002) Chondrocyte damage following osteochondral grafting using metal and plastic punches: comparative study in an animal model. J Orthop Surg (Hong Kong) 10:170–172
Outerbridge R (1961) The etiology of chondromalacia patellae. J Bone Joint Surg Br 43:752–757
Rinaldi E (1982) Treatment of osteochondritis dissecans and cartilaginous fractures of the knee by osteo-cartilaginous autografts. Ital J Orthop Traumatol 8:17–21
Sanders TG, Mentzer KD, Miller MD, Morrison WB, Campbell SE, Penrod BJ (2001) Autogenous osteochondral ``plug'' transfer for the treatment of focal chondral defects: postoperative MR appearance with clinical correlation. Skeletal Radiol 30:570–578
Schottle PB, Oettl GM, Agneskirchner JD, Imhoff AB (2001) [Operative therapy of osteochondral lesions of the talus with autologous cartilage-bone transplantation]. Orthopade 30:53–58
Siebert C, Miltner O, Weber M, Niedhart C (2001) Einwachsverhalten von osteochondralen Transplantaten–eine tierexperimentelle Studie. Sport Orthop Traumatol 17:120
Steadman JR, Rodkey WG, Briggs KK (2002) Microfracture to treat full-thickness chondral defects: surgical technique, rehabilitation, and outcomes. J Knee Surg 15:170–176
Sternberger LA (1969) Some new developments in immunocytochemistry. Mikroskopie 25:346–361
Tibesku CO, Szuwart T, Kleffner TO, Schlegel PM, Jahn UR, Van Aken H, Fuchs S (2004) Hyaline cartilage degenerates after autologous osteochondral transplantation. J Orthop Res 22:1210–1214
Wagner H (1964) Operative Behandlung der Osteochondrosis dissecans des Kniegelenkes. Z Orthopädie: 62–64
Yamashita F, Sakakida K, Suzu F, Takai S (1985) The transplantation of an autogenetic osteochondral fragment for osteochondritis dissecans of the knee. Clin Orthop: 43–50
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rose, T., Craatz, S., Hepp, P. et al. The autologous osteochondral transplantation of the knee: clinical results, radiographic findings and histological aspects. Arch Orthop Trauma Surg 125, 628–637 (2005). https://doi.org/10.1007/s00402-005-0010-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-005-0010-8